Since the start of the pandemic, healthcare workers have carried the heaviest burden. Especially those who are immunocompromised while working in harm’s way. This week on Lights, Camera, Crohn’s you’ll hear from three healthcare workers with IBD who are immunocompromised and have received their first vaccine. It’s my hope that by hearing from these warriors firsthand that you’ll gain a sense of comfort, understanding, and perspective while also understanding the importance of debunking medical misinformation. Our IBD community is delicate and requires more expertise than simply listening to a family member or friend who “read something on the internet” or someone who has a cousin with Crohn’s (or now COVID).
Wearing several hats—IBD Mom and Relief Charge RN in COVID Unit
When Shermel Edwards-Maddox of Houston was diagnosed with Crohn’s disease in 2007 at age 24, little did she know that she’d one day lead the charge in a medical unit in the thick of a pandemic, while having two kids and a husband at home, while being on a biologic.
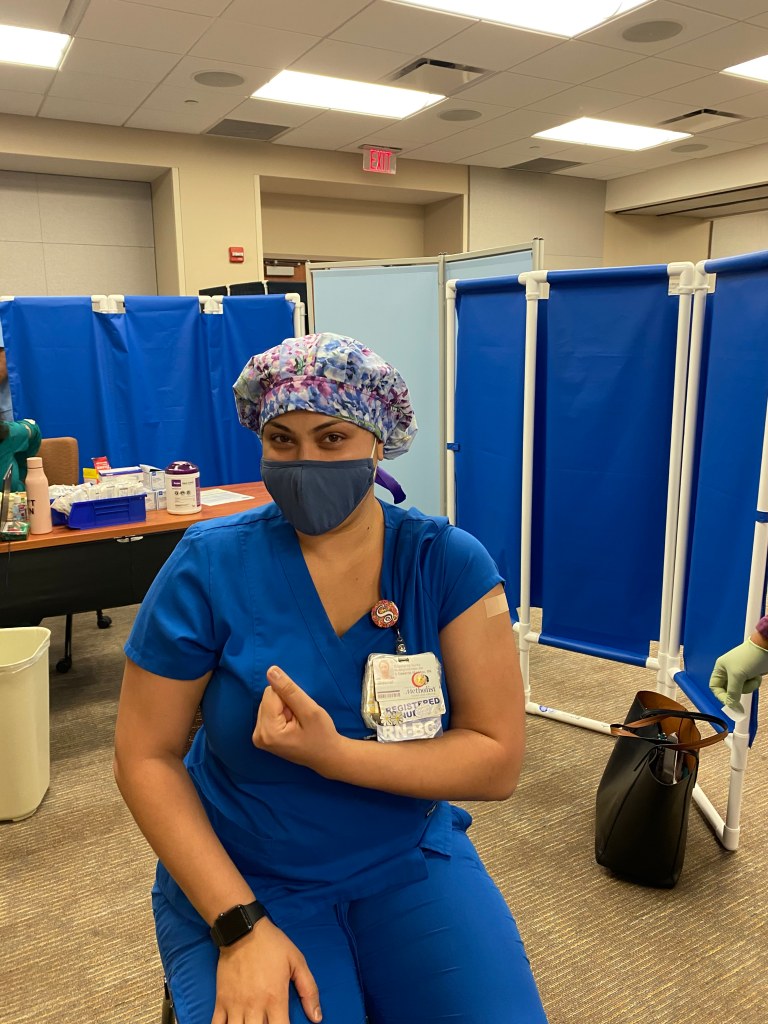
“It has been both physically, mentally, and emotionally draining. I imagine that every healthcare worker has been afraid however being immunocompromised has added an extra layer of fear. The emotional and mental exhaustion comes from the constant worry of “what if today is the day I catch COVID”? Every time I step onto the nursing unit, I’m aware that I could contract the virus. It’s very reminiscent of IBD and the worry of whether a flare is starting.”
Like many other healthcare workers (and the general population for that matter!), she says the roll out of the vaccine provided her with a sense of relief, but also an understanding about the importance of educating the public about the importance of getting vaccinated. As a nurse, she has a solid understanding of how clinical trials work and knows that more than 70,000 people received the vaccine between the Pfizer and Moderna trials. She was especially excited to receive the vaccine after it was found to be 95% effective. Shermel feels blessed to receive “0.3ml of hope” in a syringe and says many in her shoes feel like they just received their “second wind” after months of being beyond exhausted.
“It was quite emotional. I shed several tears in the days leading up to the vaccine. Those tears were in amazement of how grateful I am to be getting a vaccine that could spare me from this horrible virus that takes the lives of so many. When it came time for getting the vaccine, I felt pure excitement!”
Shermel’s only side effect she experienced was a sore arm, which is expected with any type of vaccine.
The COVID vaccine allows Shermel to not only protect herself but her husband, children, patients, and the community. It makes her feel hopeful to know her daughter will get to see her kindergarten teacher’s face without a mask and that her son will be able to attend his school graduation, free of social distancing.
From an Ostomy Reversal in March to working as a clinical researcher
Caroline Perry also happens to live in Houston and after battling Crohn’s since the age of eight in 2000, she had an elective ostomy reversal surgery March 4th just as the pandemic was unfolding in the States. She takes Entyvio AND Stelara and says that even though she’s on two biologics, her physician had explained to her that both drugs have a relatively good safety profile. While she wasn’t overly nervous about contracting the virus more than the next person, she has been nervous about how her body would react to it.

As a clinical researcher, her boss, happens to be her gastroenterologist. Having her care team readily available and working alongside people she knows and trusts on both a personal and professional level has helped her cope through the pandemic immensely.
Prior to receiving the vaccine in December (2020), Caroline admits she had some initial concerns and brought them up to her doctor, which is what she recommends everyone does.
“Many people are getting all their information from the internet or by word of mouth and are neglecting to listen to our experts—some even mistrusting them. My doctor gave me lots of evidence on why she believes the vaccine is safe and debunked a lot of my fears, which I found out were fairly common questions or misconceptions regarding the vaccine. I got the information I needed to make an informed decision, and once I had all the information, I was no longer worried about getting the vaccine! I am much more concerned about getting COVID than any potential side effect of its vaccine.”
Caroline says she was so excited to receive the vaccine, not only for herself, but for all the healthcare workers that were in the room with her.
“Sitting in that chair, it hit me. I was really experiencing a significant piece of history and I will never forget the feeling of palpable relief in that room. As healthcare workers, we have heard nothing but bad news for so long, and the vaccine is a beacon and glimmer of hope, at the end of a very long tunnel.”
Due to the pandemic, Caroline and her fiancé canceled their wedding for the time being, but finally feel like they can breathe a sigh of relief. Her fiancé won’t be eligible to receive the vaccine until the last round is available, so until then, she says they will continue to practice COVID precautions and keep up to date with the latest data surrounding the vaccine.
After receiving the vaccine, Caroline still received her Entyvio that afternoon! Her only side effect, like Shermel, a sore arm. As of now, she’s working on COVID research in addition to her usual IBD research. Caroline says this past week was her first time working in the COVID ICU for a new clinical trial, and she felt a lot safer thanks to having the first vaccine.
Juggling Women’s Health while being a mom of 3
Janice Eisleben, a Women’s Health Nurse Practitioner in St. Louis, was diagnosed with Crohn’s in October 2017 while pregnant with her third child. She was initially on Humira, but started Stelara a year ago. Janice happens to work at the OB office I go to, so I know her personally and have experienced her amazing care through my own pregnancies. We connected immediately once we both discovered years ago that we were IBD moms on biologics.

She recalls how scary the onset of the pandemic was, between the limited information and the looming unknown. As a patient with IBD, on a biologic, she wasn’t sure what that ultimately meant for her well-being. When she found out the vaccine was going to start being available to healthcare workers, Janice says she was elated.
“I feel like the vaccine finally offers some level of comfort to healthcare workers who have literally been giving everything they have to take care of patients. And this is not limited to nurses and doctors! The hospital cannot run without the respiratory therapists, housekeepers, and maintenance staff—these people are truly the unsung heroes of this pandemic.”
Janice said she did not have concerns or worries about the vaccine because she had been following the clinical trials from the early stages. She says the energy she felt just standing in line to receive her vaccine was something she’ll always remember and that everyone there was beyond ready to take this next step.
“It was incredibly emotional. I honestly teared up when I received the email inviting me to schedule my appointment. I was so excited that the night before I had trouble sleeping—kind of like a kiddo who can’t sleep the night before Santa comes. This vaccine means so much for us. It means that maybe sooner than later I will feel more comfortable with my kids going back to school and participating in activities. It means that we have less worry about me bringing this virus home from work to our household, and less worry about me getting a severe case of this virus.”
She says she can completely understand why someone would be skeptical of the vaccine, but she encourages everyone to avoid the “Google trap” and to please contact your physicians/care providers to discuss it further. For anyone with IBD, Janice advises you to specifically contact your gastroenterologist. If there is anyone those of us with Crohn’s and ulcerative colitis should trust, it should be our GI!
Janice’s only side effect was also a sore arm, though she does anticipate more symptoms (low grade fever, aches, fatigue) after the second dose, because this was well documented in the trials.
Helpful Resources to Educate Yourself About IBD + COVID Vaccine
About IBD: Podcast Interview with Dr. David Rubin: A Key Opinion Leader in IBD Helps Patients Understand What to Expect with Vaccination
Crohn’s and Colitis Foundation: COVID-19 Vaccines: What IBD Patients & Caregivers Need to Know




















