If you’re a young girl or woman diagnosed with a chronic illness, prior or during your “childbearing” years, chances are you or your parents may wonder what this means for your future family. When I was diagnosed with Crohn’s disease at age 21 in 2005, the thought of settling down and having kids was not on the radar but ever since I was a little girl I always aspired to be a mom. Fast forward to 2008, I was hospitalized for an abscess and taken off Mesalamine and put on a biologic injection (Humira). I can still picture the discussion with my GI. My mom sitting on the couch alongside the hospital window, looking at me wide-eyed, and us wondering if I’d ever be able to have children on my new medication. A medication I was told I’d be on for the rest of my life. I was 24. Back then there was nowhere near the research or guidance available like we have today.

It was the first time I really began to question and worry about whether I’d physically be able to be a mom. As the flare ups, ER visits, hospitalizations, and tests persisted for years, I honestly didn’t have the energy to think about what my life would look like down the road, I only had the energy to focus on what was going on in that moment. I was not a patient advocate and looking back I was a bit naïve and uneducated about what it meant to have not reached remission.
When I met my husband in 2013, little did we know that for the next two years I would be at my sickest. What we did know—is that we both wanted kids one day. After my third bowel obstruction hospitalization in 15 months, I needed bowel resection surgery in August 2015, which FINALLY put me into surgical remission. Ironically, I was engaged to be married. Babies were on the brain. Since I lived a decade without remission, we knew we were going to have to try for a baby as soon as we got married, as remission can be fleeting. At 32 years old, I didn’t want to take any chances.

A lot has happened since we got married. We got pregnant a month after getting married. Lost our second baby around 7 weeks. And then had our rainbow baby in 2019 and our caboose of the family in 2021. If you’ve followed my advocacy and blog, you know I’m passionate about showing all that’s possible despite your IBD. I know each of our journeys is incredibly intricate and unique, each of us deals with our own set of challenges. But I also know that my younger self would have benefited immensely from seeing and hearing fellow women who’ve been there and done it and have families to show for it despite their chronic illness.

This week on Lights, Camera, Crohn’s we hear from several IBD moms—with kids ranging from newborn age to now adults—who offer amazing perspective that I hope will make you feel comfort in what the future could hold for you.
What IBD moms want you to know
Jennifer: “It’s 100000000 percent worth it! And be honest with your kids and spouse about how you are feeling and what you are going through. Of course, make it age appropriate, but they need to know the struggle.”
Liz: “Your kids will learn their limits and love on you when you need rest. It’s ok to go slow. Even if you flare after birth, you will come out of it.”

Amber: “I would tell a younger me that my body WAS capable of carrying and delivering healthy BIG (lol) babies. After struggling with fertility and then conceiving twins and carrying them full-term, I realized my body hadn’t failed me (how I think so many of us with IBD feel. Motherhood is possible for us and thank you Natalie for reminding us of that.”
“Find your people and be honest with them about how you are doing. Don’t ever feel bad asking for help. It truly takes a village to help.”
Brooke: “One day, you will be better. One day, you will coach little league and make the playoffs. One day, you will work on Capitol Hill. One day, you will live in another country. One day, you will be the best mom and you will thrive through IBD. You’re almost there!”

Jaime: “I would tell my younger self that fertility is not something you take for granted especially with a chronic inflammatory disease that can leave you prone to developing scar tissue. I’d also tell her that IBD may make life hard for awhile but with the right doctors, life will improve and the family you dreamed of having will happen.”

Jessica: “Motherhood is hard. It’s ever harder when you have an illness. It’s ok to rest when needed without feeling guilty.”
Kaitlyn: “Your kiddos are more resilient and adaptable than you think they are. I had a major flare about 7 months after my son was born. I put off being admitted to the hospital for weeks because I was so scared and felt guilty for leaving my baby and thinking he would feel abandoned without any way to explain to him that I was gone. He ended up having a blast with my husband for a week and I finally was able to achieve some sense of relief (slowly coming out of that flare, but there is a light at the end of the tunnel). Also, you’re not a bad mom for not being able to do the things you think you should be able to do (Spoiler Alert: Your baby doesn’t know other moms take their babies on long walks around the park and don’t have to drag you into every public bathroom you pass while running errands).”
Patti: “You only get one chance to raise your babies, so don’t sweat the small stuff. And frequently remind yourself (on the roughest days) that you really ARE doing the absolute best you can…and that is OKAY.”
Alyssa: “Sometimes you’ll be holding your baby on the toilet, but you’ll be okay, and your baby will be okay. The road will be tough, but so worth it. Some days the kids will watch more TV than you want, but you must take care of yourself too so you can be present for them. They’re resilient and will love you no matter what.”

Ally: “Rest when you can! Your body will most likely go into remission once pregnant so not need to get scared or nervous about it.”
Liv: “Make yourself and your health a priority. I went into a huge flare after having my first baby because I was SO focused on her and not eating properly or showering or taking care of me. Meal prep to make the mental load of eating easier! And ask for help!”
Patra: “Don’t be so hard on yourself when you feel the need to rest.”
Phoebe: “I would tell her to follow Natalie Hayden’s blog and IG account (haha)…seriously though, when I see you and other people share about their pregnancies and family life, it gave me hope to have my child. I would also tell my younger self it’s ok if you’re a mom with chronic illness! My younger self assumed I had to have a perfectly healthy body to have babies and raise babies.”
“Take care of yourself, even if it means asking your loved ones to look for signs of your anxiety and exhaustion that you may just be trying to push through or ignore.”
Jenni: “I would tell myself not to be so hard on myself. I would say don’t take on all the sick mom guilt. To let them watch movies and eat cereal without stressing about it when I wasn’t feeling well. I would also say…you don’t have to pretend to be brave all the time. It’s ok for them to see you cry or feel frustrated or be sick. They can handle it, and it is creating such strong, caring, empathetic humans!”
Courtney: “I would tell my younger self that I am enough for my kids and that they will be better people because of what they learn and see.”
Mallory: “Your children are strong, and they understand that it’s not your fault.”
Meg: “You did the right thing by staying on your meds through pregnancy and your baby is perfect.”
Kelly: “You are enough. Don’t feel like you’re not able to be as great of a mom as a healthy mom is.”
Ryann: “All you need is love. While I’m sure my son loves the active days when we’re doing lots of activities, he’ll be fine on the days that I’m laying down on the couch as long as I show him love.”
Rachel: “You’re stronger than you know, and everything will work out no matter what happens.”
Amanda: “Not to let fear of the “whatifs” cripple you.”
Brenda: “You will do great and be sure to find a selfless hands-on partner.”
Kristin: “Give yourself some grace. I didn’t get diagnosed or have any Crohn’s issues until my son was 15 months old. The symptoms came on like wildfire and it took a village to help until I figured it all out.”
Anna: “I want to jump in this convo as a 50 year old who wanted to be a mom, but due to the severity of my disease (diagnosed at 18), was told at 29 to have children by 35 due to being high risk and at 34, I was told not to carry due to complications and unfortunately adoption was not in my future as a single woman with severe illness no another option (freezing eggs, etc.) at that point in time. I feel like that is the MAIN thing Crohn’s stole from me! After many years of therapy, I cope with it very well now; however, I still from time to time mourn not being able to have children that aren’t four-legged…#dogmama!”
Courtney: “I would tell my younger self not to worry about having to use the bathroom urgently so much and that you’ll be carrying around diapers, wipes, and a little potty in your car for years. Your kids will also be able to relate to having accidents. I would all tell her that fertility declines a lot faster for people with chronic inflammation and to get your AMH levels checked early. Or think about freezing embryos if you want a big family in your mid to late thirties. Lastly, that breastfeeding won’t stop your kid from having IBD, so don’t worry about giving them formula.”

Ashley: “So, one time I posted on Reddit about how I have ulcerative colitis and didn’t know if I should have kids…I got a lot of responses. I got 56 that told me not to do it. How they were miserable. Or how their mom had it and they suffered as a kid. It was honestly traumatizing. And int that moment, I made the decision not to have kids.”
Tricia: “There will be some really tough days with your illness, and trying to take care of your kids, but you’ll get through this, and better days are ahead.”
Shannon: “Nap when the baby naps is legit. But also, when the baby is 12, you’re still going to need to take a nap. And that’s okay. It doesn’t make you less than because your body requires rest and reset. It is productive to take a nap if it’s necessary.”
Chanel: “That this chronic illness has a direct effect on pregnancy. Having this disease since 7 years old, no doctors ever thought it would be helpful to mention how important being in remission was before getting pregnant or trying for a baby until I was 26 years old and happened to nonchalantly mention to my doctor at the time that we were going to start trying.”
Jennifer: “Don’t worry! You will be blessed with two beautiful children and IBD will not define who you are and will not hold you back from anything!”
Stephanie: “Be easy on yourself and don’t put high expectations on yourself. It will all be worth it. Take it a day at a time and do what you need to do to feel better. Your kids will learn and be more empathetic and compassionate people for it.”
Bhavna: “It’s going to be hard. More emotionally than physically. You will even doubt whether you should have kids for fear of passing it on. I know eventually I did. My daughter now has an autoimmune condition. But despite all of this, you will make it through. Stronger. Resilient. Sometimes a tad sadder.”
Rosanne: “Kids are more resilient than you think. Motherhood is worth having to potentially miss a few things because of a flare or a difficult day. Your kids will understand and be stronger because of it.”
Pie: “Mum guilt will chew you up on the days that you can’t get out of bed. It’s okay, your little one will grow up to be empathetic and understanding of others.”

Amy: “I was completely well for the 8 years I was pregnant and breastfeeding my three boys. Almost a year after finishing feeding my youngest, I immediately went into a massive flare and have not managed to recover yet (10 months now). I felt betrayed all over again by my body, just at the time when I needed it to be strong. I would tell her that the most important thing is that you’re well, so that you can be the best version of yourself. Children are beautiful, they will take you exactly as you. Try to follow their lead. You are enough. They will forget at times you were absent due to resting, appointments, etc. But they will remember how hard you fought for your health. My middle school boy now seems to be suffering with gastro issues and it’s essential to me that I show him that I have the disease, it does not have me (enough though some days that doesn’t quite work out).”

Megan: “Some days are hard, but you can do it! You will be shocked at how much compassion it gives your children. They understand “mommy doesn’t feel well” at such an early age and really want to help take care of us. Vivi asks me daily, “Mommy, does your belly hurt today?” and says, “I’ll take care of you, Mommy.”
Kara: “Don’t forget to take care of you before it’s too late! You are doing your best and your children will only remember that later. My kids are 8 & 10 now, but when I was pregnant with my youngest, I went into a flare and refused to tell anyone or acknowledge it, thinking it would make me a bad/weak mom…so dumb right? By the time my youngest was 1, I was making an appointment for a temporary ileostomy bag. But my kids only remember the sweet stuff.”

Stephanie: “Simply, it’s possible! It was worried for so long that it wasn’t possible, especially once on a biologic and your Instagram page, Natalie, gave me so much hope! Now, less than 2 weeks from delivering my second baby (but my first pregnancy on a biologic).”
Marnie: “I would tell my kids your disease becomes part of your everyday routine, but it doesn’t define you.”
Crystal: “Make sure your baby learns to take a bottle in case you end up in the hospital with a flare.”
Leslie: “Don’t be scared to be on all the medication you need. You’ll get pregnant one day like you always dreamed.”
Keyla: “This journey will be hard but no matter what your little one becomes stronger through it with you.”
Christine: “Here I am celebrating my 47th birthday with my teenagers! One of the first questions I asked my doctor, according to my mom, was will I be able to have kids? That was when I was 23 years old. Here I am at 47, and they have seen me at my best, and unfortunately, my worst. They are truly the reason why I keep going and want to keep fighting at the worst of times.”

Amy: “Your journey might look different than others, but you can still have a family. Also, accept help when you need it.”
Robin: “My kiddos are 27 and 25 now and I was diagnosed when the 27-year-old was 2.5 and the 25-year-old was a baby. She turned one and took her first steps in the family visiting room at the hospital. So, I have the benefit of living with the fruits of my parenting labor. My IBD has taught me that life is precious. Each moment is precious. Because of this, I really tried to take advantage of life when I was feeling well. AND ALSO, I tended to push through when I wasn’t feeling well if something was important to my family, specifically my children. Your first instinct as a parent will be to protect your children from what you are going through – but it’s ok to be open about what you are experiencing in age-appropriate ways. There is no one perfect way to be a parent, much less be a parent with a chronic illness. Give yourself some GRACE.

If dads, or aunts, or family friends, or grandparents are jumping in to chauffeur your kiddos and/or take them to do fun things that you can’t do – IT STILL COUNTS! Your kids are still getting to do the thing. Your kiddos will benefit from having other adults they know and trust in their lives.
Parenting isn’t for the faint of heart. Connect with people that can share the burden. It’s ok to ask for help. I write this while remembering my mantra was “suck it up and figure it out” when they were little. Granted – I was a single parent for a lot of their young life, and I was fortunate to have a strong support system. Even with the support it was difficult to ask for help. SO, ASK FOR AND ACCEPT HELP.
I don’t know what kind of mom I would have been without IBD, but based on who my girls are now, I’m ok with the mom I was and am with IBD.”
Final Thoughts
Hearing this firsthand perspective from all these incredible IBD moms is so inspiring and comforting. It’s a reminder we are not alone in our struggles or our fears—and let’s face it, motherhood isn’t all sunshine and rainbows. But the beauty motherhood brings to our lives and the unbelievable love you feel for your children is the sunshine and the rainbows that makes it all worth it. When you’re an IBD mom, yes there’s a lot of internalized pain and worry. But there’s also so much motivation and joy found in looking into the eyes of your children and knowing that you are enough and will always be enough for them because you’re you.

There are times when their diapers and bathroom habits may set off alarm signals in your head. Don’t think I haven’t brought one of my kids to the ER because I was fearful, they had IBD…wasn’t that. There have been moments where I’ve been bent over making school lunches. There are times I’m on the couch with a heating pad during bedtime stories or in the bathroom mapping out my game plan of how life will go on if I’m hospitalized, and all the moving places I have to orchestrate if I’m out of commission. But SO much overshadows those moments.
As an IBD mom of three, my kids give me such purpose to celebrate each day and soak in each experience I’m blessed to share with them. They provide me with renewed faith in my body and all that I’m capable of. They remind me to laugh and not take life so seriously. When I’m in pain or going through prep for a scope or an uncomfortable procedure my thoughts float to their sweet faces and the incredible memories we’ve shared and it’s the best reprieve from my painful current reality.
When you’re a mom with chronic illness, sure the days can feel long and the years short…but you have a different level of gratitude for what may seem mundane to others. You will second guess yourself more than your children ever will. They are sponges, watching and soaking up their lived experience with you and without even doing anything you’re raising a children with innate empathy and compassion that you’ll see play out as they grow up—I’ve seen it for YEARS with my kids—and while I wish they weren’t the way they are because of my health, I also wouldn’t have it any other way. IBD is a family disease, it impacts way more than just the patient and know that if you choose to carry children, adopt children, or have babies through surrogacy, you are never a burden to your family. You are enough and always will be to your beautiful babies.
My family planning advice for you
My advice family planning
- Have the discussion about your future 3-5 years out (if possible) so you can get a game plan in place. Something as simple as letting your provider know…”someday I hope to be a mom”…is sufficient. This sets the stage for what makes the most sense medication wise, targeting and tracking remission, planning scopes so you can get the ‘green light’ before conception, etc.
- Do not try and conceive if you haven’t been in remission for at least 3-6 months. Sure, pregnancies are not always planned and can be a surprise but try not to get pregnant while you’re flaring or have active disease as that increases the likelihood of flaring during pregnancy and after delivery.
- Once you find out you’re pregnant, alert your GI the same day as your OBGYN and get the ball rolling on finding a maternal fetal medicine (high risk OB) to be part of your care team.
- Do not try and go rogue and go off all medications for pregnancy. Talk with your care team. Do the research so you can see firsthand about the safety and efficacy of most IBD meds in pregnancy and breastfeeding and be confident that by keeping yourself well and your disease controlled in pregnancy, you are helping you and your baby.
- Check out the PIANO study and MotherToBaby research opportunities so you can help pave the way for future IBD moms and contribute to research. It’s so rewarding, and your voice and input makes a world of difference. My older two were part of MotherToBaby studies and my youngest is part of PIANO, he’s being “followed” until age 18!
- Never hesitate to reach out to fellow women with IBD on social media who are moms and receive firsthand advice about their journey so you can feel a bit more at ease about yours.





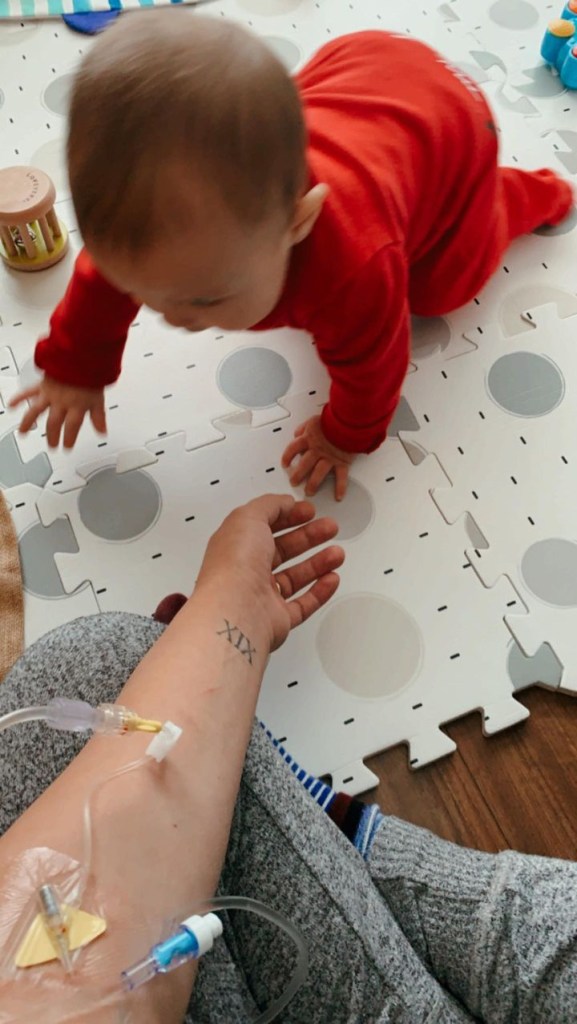


















































 Addy’s son, William, is now 13 months old. This week—she shares a guest post about her journey to bring him into this world and the challenges and victories she’s experienced as a new mom with IBD. I’ll let her take it away.
Addy’s son, William, is now 13 months old. This week—she shares a guest post about her journey to bring him into this world and the challenges and victories she’s experienced as a new mom with IBD. I’ll let her take it away.
 After my second-high blood pressure reading that week, a nurse advised me to come into labor and delivery. When I arrived, I was diagnosed with gestational hypertension and started the induction process the next morning at 37 weeks.
After my second-high blood pressure reading that week, a nurse advised me to come into labor and delivery. When I arrived, I was diagnosed with gestational hypertension and started the induction process the next morning at 37 weeks. When William was born, I was thrilled, and so fortunate, to have a successful early breastfeeding relationship with him. When I started flaring again, breastfeeding became a significant challenge. I’d be with William during a late-night feeding, get a few minutes in, then have to wake my husband to keep William safe while I quickly ran to the bathroom. Obviously, this made William more than a little upset to start eating only to be pulled away. I also became increasingly worried that he wasn’t getting the nutrition he needed from me because I wasn’t absorbing nutrients the way I needed to. I upped my supplements and kept close tabs on his weight but continued breastfeeding. At this point, I knew I needed to do something different with my medications. What I was doing clearly wasn’t working.
When William was born, I was thrilled, and so fortunate, to have a successful early breastfeeding relationship with him. When I started flaring again, breastfeeding became a significant challenge. I’d be with William during a late-night feeding, get a few minutes in, then have to wake my husband to keep William safe while I quickly ran to the bathroom. Obviously, this made William more than a little upset to start eating only to be pulled away. I also became increasingly worried that he wasn’t getting the nutrition he needed from me because I wasn’t absorbing nutrients the way I needed to. I upped my supplements and kept close tabs on his weight but continued breastfeeding. At this point, I knew I needed to do something different with my medications. What I was doing clearly wasn’t working.


 studies suggest it may start with a bacterial imbalance in the gut, and several studies have shown that people with IBD were less likely to have been breastfed as infants. Furthermore, a study in Denmark showed that breastfed babies developed certain types of healthy bacteria in their digestive tract, which non-breastfed babies were lacking. A healthy amount of beneficial gut bacteria can promote a healthy immune system which fends off different diseases.
studies suggest it may start with a bacterial imbalance in the gut, and several studies have shown that people with IBD were less likely to have been breastfed as infants. Furthermore, a study in Denmark showed that breastfed babies developed certain types of healthy bacteria in their digestive tract, which non-breastfed babies were lacking. A healthy amount of beneficial gut bacteria can promote a healthy immune system which fends off different diseases. It wasn’t easy, but I’m so glad I stuck with it. We lasted 16-months until he self-weaned and he has a very healthy immune system so far, despite the cesarean and me being on Humira. Best of all? I didn’t have a postpartum flare, which my doctor attributed to the combination of staying on my medications, following my diet plan and breastfeeding.
It wasn’t easy, but I’m so glad I stuck with it. We lasted 16-months until he self-weaned and he has a very healthy immune system so far, despite the cesarean and me being on Humira. Best of all? I didn’t have a postpartum flare, which my doctor attributed to the combination of staying on my medications, following my diet plan and breastfeeding. as possible, especially in the first 24 hours, and provide plenty of skin-to-skin. After a c-section, the last thing I wanted to do was constantly get in and out of bed to pick up a newborn. Instead, I just spent my days with my son nestled on my chest so we could both sleep, heal, bond and get my milk flowing.
as possible, especially in the first 24 hours, and provide plenty of skin-to-skin. After a c-section, the last thing I wanted to do was constantly get in and out of bed to pick up a newborn. Instead, I just spent my days with my son nestled on my chest so we could both sleep, heal, bond and get my milk flowing. Cut yourself some slack. Becoming a mother is stressful, but if you are feeling overwhelmed, talk to someone. Postpartum depression and anxiety are very real and as a mother with chronic illness, you may be more prone to those feelings. Seek out help from your spouse/partner, enlist nearby family/friends for support, and keep in close contact with your doctor to manage your symptoms.
Cut yourself some slack. Becoming a mother is stressful, but if you are feeling overwhelmed, talk to someone. Postpartum depression and anxiety are very real and as a mother with chronic illness, you may be more prone to those feelings. Seek out help from your spouse/partner, enlist nearby family/friends for support, and keep in close contact with your doctor to manage your symptoms.