For many women, living with chronic illness means constantly decoding what our bodies are trying to say. When you have inflammatory bowel disease (IBD), whether Crohn’s disease or ulcerative colitis, you get used to tracking symptoms, identifying triggers, and advocating for yourself.
But what happens when something doesn’t quite fit the IBD pattern and the usual narrative?
For a significant number of women, the answer may be endometriosis, a condition that often overlaps with IBD in ways that can delay diagnosis, complicate treatment, and intensify daily life. This week on Lights, Camera, Crohn’s we break down the possible connection, what to watch for, and how to advocate for the care you deserve. I don’t personally have endometriosis with my Crohn’s, so you’ll hear from 10 women who live this reality as they transparently share what it’s like for them and what they’ve learned along the way.

What Is Endometriosis?
Endometriosis occurs when tissue similar to the lining of the uterus grows outside the uterus. This can happen on the ovaries, fallopian tubes, bowel, bladder, and other pelvic structures. This tissue still responds to hormonal cycles, which can lead to:
- Inflammation
- Pain
- Scar tissue (adhesions)
- Organ involvement (including the intestines)
I ran a poll in my Instagram Stories asking about IBD and endometriosis. Of the 85 votes, 27% of women said they have both, 31% said they think they may have both, and 42% said they don’t have both. Those numbers speak volumes.
What the Stages of Endometriosis mean
Endometriosis isn’t staged the same way cancers are, it’s not about how dangerous it is, but about how much disease is seen during surgery. The most used system is from the American Society for Reproductive Medicine, which divides endo into four stages based on location, depth, size of implants, and scar tissue (adhesions).
Here’s what each stage means:
Stage I — Minimal
- Small, superficial patches of endometrial-like tissue
- Little to no scar tissue
- Often found on the ovaries or pelvic lining
What it feels like:
Symptoms can be mild… or surprisingly intense. Some people with Stage I still have significant pain.
Stage II — Mild
- More lesions than Stage I
- Some may be deeper (not just surface-level)
- Minimal adhesions may start forming
What it feels like:
Pelvic pain, painful periods, sometimes pain with ovulation. Still very variable.
Stage III — Moderate
- Many lesions, including deep implants
- Presence of adhesions (organs may start sticking together)
- Small cysts on ovaries called endometriomas may appear
What it feels like:
More consistent pelvic pain, possible pain with sex, bowel symptoms depending on location.
Stage IV — Severe
- Extensive deep lesions
- Thick adhesions (organs can be significantly stuck together)
- Larger ovarian endometriomas (“chocolate cysts”)
- May involve bowel, bladder, or other organs
What it feels like:
Chronic, often severe pain; higher likelihood of fertility challenges; symptoms tied to whichever organs are affected.
The most important thing to understand
Stage does NOT equal pain level. Someone with Stage I can be debilitated, while someone with Stage IV might have fewer symptoms. That’s one of the most frustrating parts of endo, it doesn’t behave predictably. That being said, just because you may have Stage 1 should not diminish your experience as a patient or the suffering you are coping with.

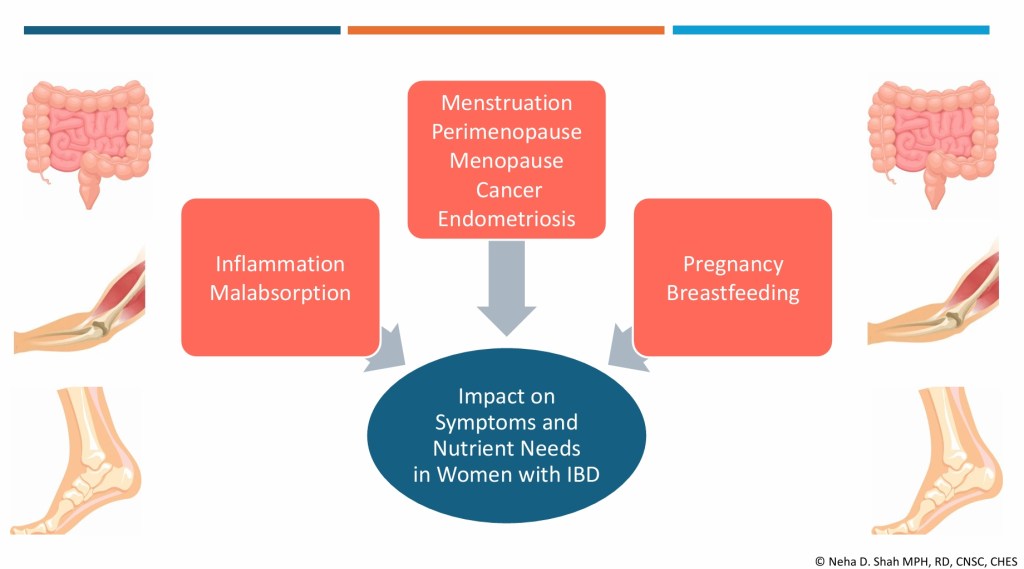
Why Endometriosis and IBD Get Confused
The overlap between endometriosis and IBD is more than coincidental, it’s believed to be symptomatically and biologically intertwined.
Both conditions can cause:
- Abdominal pain and cramping
- Diarrhea or constipation
- Bloating
- Fatigue
- Nausea
- Pain with bowel movements
If you already have IBD, it’s easy to assume these symptoms are just part of a flare.
Hormonal Influence
Endometriosis is hormone-driven, meaning symptoms often worsen:
- Before or during your period
- Around ovulation
Some women with IBD also report symptom fluctuations tied to their menstrual cycle, which can blur the lines even further.
Inflammation Connection
Both conditions involve chronic inflammation, and emerging research suggests there may be shared immune pathways. Women with IBD may have a higher likelihood of developing endometriosis—and vice versa.

Red Flags That It Might Be More Than IBD
If you’re living with IBD, here are signs that something else, like endometriosis, could be at play:
- Pain that follows your cycle (gets worse before/during your period)
- Severe pelvic pain that feels different from your typical IBD pain
- Pain during or after sex
- Pain with bowel movements specifically during your period
- Infertility or difficulty conceiving
- IBD treatments aren’t improving certain symptoms
One of the biggest clues? When your gut symptoms don’t fully respond to your usual IBD medications.
The Diagnostic Challenge
Diagnosing endometriosis isn’t straightforward.
- Imaging (like ultrasound or MRI) can help, but may miss smaller lesions
- The gold standard is laparoscopic surgery, where a specialist can see and biopsy the tissue
For women with IBD, this can feel overwhelming, especially if you’ve already been through scopes, scans, surgeries, and procedures. But getting clarity matters.

How It’s Treated
Treatment depends on severity, symptoms, and your goals (like pain relief vs. fertility).
Hormonal Therapy
- Birth control pills, patches, or IUDs
- Medications that suppress estrogen
These aim to reduce or stop the growth of endometrial tissue.
Pain Management
- NSAIDs (with caution in IBD, especially Crohn’s)
- Other pain-modulating medications
Surgical Treatment
- Laparoscopic excision of endometriosis lesions
- Particularly helpful for more advanced disease
Coordinated Care
If you have both IBD and endometriosis, your care team may include:
- A gastroenterologist
- A gynecologist (ideally one who specializes in endometriosis)
- A colorectal surgeon if bowel involvement exists
This team-based approach can make a huge difference.
Living With Both: Practical Advice
Track Your Symptoms Differently
Don’t just track food and bowel habits. Be mindful of:
- Your menstrual cycle
- Pain timing and location
- Symptom patterns across the month
Patterns can reveal what labs and scans can’t.
Don’t Dismiss “New” Pain
You know your IBD. If something feels different, it probably is. Trust that instinct.
Be Specific With Your Doctors
Instead of saying “I have more pain,” try:
- “This pain is worse during my period.”
- “It feels lower in my pelvis than my usual Crohn’s pain.”
- “My GI symptoms spike even when my inflammation markers are normal.”
Details help providers connect the dots faster.
Be Careful With Medications
Some common treatments for one condition may complicate the other:
- NSAIDs can aggravate IBD
- Hormonal treatments may affect GI symptoms differently for each person
Always loop in both your GI and GYN teams.
Advocate for a Second Opinion
Endometriosis is often underdiagnosed and misunderstood. If you feel dismissed, it’s reasonable to seek a specialist, especially one experienced in excision surgery, not just symptom management.

The Emotional Side No One Talks About
Living with one chronic illness is hard enough. Adding another, especially one that affects fertility, hormones, and daily pain, can feel overwhelming.
There’s often:
- Frustration from delayed diagnosis
- Anxiety about symptoms overlapping
- Exhaustion from managing multiple specialists
If this is your reality, you’re not alone and you’re not imagining it.
The Patient Experience: What women with IBD and endometriosis want you to know
Madison: “I could write a novel about endometriosis and IBD! I’ve had three surgeries for endometriosis, and it’s been found on my bowel in two of the surgeries. I eventually asked my GI if it could have been endo all along (it’s not), but it’s interconnected.
She was diagnosed with ulcerative colitis in 2016 but had symptoms for a few years prior. Madison was diagnosed with endometriosis in August 2020 after unexplained infertility but more importantly, debilitating pain once she stopped birth control in early 2019. Looking back, she says her symptoms probably started at puberty (12 years old) but she didn’t know what was normal.
“I had surgery in August 2020 to confirm the endometriosis diagnosis and have had 2 additional surgeries since then. I wish I would have known during my first surgery that there’s a difference between an ablation of the endometriosis and an excision of the endometriosis,” she explains. “The best way I’ve had it explained to me is imagine burning weeds in your yard vs pulling them out by the root — if you burn the weeds, they will come back. You need to pull them out by the root. However, not every surgeon is trained in excision and the recovery is definitely longer! I looked into endometriosis advocacy groups like Nancy’s Nook (Facebook) to help learn more about the differences and find excellent surgeons.”

Madison ended up having a hysterectomy in 2023 after they suspected adenomyosis (where endometrial tissue grows within the muscle of the uterus) and the quality of life she has now is significantly improved! She still has endometriosis (there’s no cure and it often regrows) but it’s managed much better now.
“I will probably have a fourth surgery in the next couple years, but I’m hopeful that the medicine and science improves to possibly delay an additional surgery. My endometriosis and my ulcerative colitis symptoms are definitely linked. If I’m in a flare for one, I tend to have symptoms increase for the other. For example, my endometriosis causes really painful bloating and I often look distended. If the distension lasts for a few days, my gut tends to revolt and I start to see an increase in GI symptoms. The last 2 surgeries showed I had endometriosis growing on the bowels (both times it was removed) so my cycles would cause really painful GI symptoms that improved after the surgeries.”
She is more convinced now that the gut/brain/pain feedback loop is real. When Madison’s endo is calm, her ulcerative colitis tends to follow suit. She’s so grateful for Instagram which has connected her to other endometriosis patients that have been willing to share their experiences.
Katherine: “Just saw an endo excision specialist 2 months ago. She wants me to do the surgery, but I’m in my second flare right now in the last year and my IBD specialist won’t sign off on it until I’m in endoscopic remission. Now dealing with fighting CVS in an appeal to increase my Rinvoq back to 45 mg.”
Katherine went on to say that one of the most vital steps in her journey was realizing that her body doesn’t operate in silos, so her doctors shouldn’t either.
“Navigating the overlapping pain of ulcerative colitis and endometriosis requires more than just two separate plans; it requires a unified front. I found that getting my IBD specialist deeply involved in my pelvic health was the catalyst for better care, especially since I noticed my symptoms would constantly peak during my cycle, creating a ‘perfect storm’ for inflammation.”
She says her GI understands the specific complexities of her UC and was able to refer her to an endometriosis specialist who wasn’t just an expert in surgery, but someone who respected the delicacy of the bowel.
“When your GI and endo specialist collaborate, you move away from ‘band-aid solutions’ and toward a strategy that addresses how these conditions trigger one another. Don’t be afraid to ask your gastroenterologist for a referral; a specialist who is already vetted by your IBD team ensures that your care plan is safe, cohesive, and designed for your specific anatomy.”
Katherine is currently in her second UC flare in six months after being in remission for five years. The plan is to start progesterone only birth control once she’s back in remission. Then she plans to get endometriosis excision surgery, and an IUD, which will help with her iron deficiency anemia.
Sabrina: “My doctors have suspected I have endometriosis, but I haven’t done the diagnostic surgery yet because I need to wait until I have my surgery to reconnect my J Pouch.”
Kelly wasdiagnosed with endometriosis stage 4 but most likely had it for years. Then, she received her Crohn’s disease diagnosis in 2005.
“We did several rounds of IVF mainly because back then it wasn’t talked about or taken seriously. I never would have done IVF because my Crohn’s got so bad. We adopted in 2009. I had my colon out in 2010. Then in 2016, I was thinking of a hysterectomy because I was so done with the anemia and pain. I ended up with a small bowel blockage due to my endometriosis and end up (I had a J Pouch—I now have an ileostomy) having an emergency hysterectomy and a 10-hour surgery to unglue all my organs and get rid of the scar tissue on my bowels and the damage from the endo.”
Kim: “I was diagnosed with Endometriosis first, then Crohn’s, then repeat scopes showed endometriosis on my colon as well. I’ve never been told there is a correlation, but it makes total sense (how women’s bodies store trauma and have far more autoimmune conditions as a result). I wish I would’ve known to advocate for myself and my symptoms as a teenager and young adult.”

Kim says too many times (especially for women) we are told it’s “normal” to have symptoms (cramps, excessive bleeding, fatigue, anemia, etc.) and as a young adult, you don’t know to challenge it.
“Even at 30 years old, my PCP was convinced my rectal bleeding was simply from hemorrhoids and only referred me to GI when I insisted. Then, that GI only performed a colonoscopy because of the referral from PCP as “IBD patients typically present much more ill” than me. We then discovered severe, chronic ulceration and full-blown Crohn’s.”
Kristin: “I was diagnosed with stage 4 endo during a hysterectomy in 2024 after years of terrible symptoms that kept me bedridden during my cycle. However, not all my symptoms were relieved from the surgery. About 15 months later (just last month), I was diagnosed with Crohn’s disease and started on biologics. For years, I was told I had a sensitive stomach, or I should take birth control. I wish I knew what endo was years ago. I also wish I knew how much more likely women with endo are for having an autoimmune disease.
Kristen wants women to know that how you describe your symptoms to doctors is just as important as what you tell them. This will directly impact testing and help in finding a diagnosis. It wasn’t until she told her GI that her symptoms were cyclical but seemed to have no rhythm or reason that the testing approach shifted. Kristen wants women to have the courage to speak up about all your symptoms, even if they seem gross or uncomfortable to talk about.
Allie: “I just wish when I was diagnosed with UC that someone would have told me the likelihood of potentially having endo and then the impact it could have on fertility. I would have gone to a fertility specialist early on and potentially frozen my eggs in early adulthood.
Kate: “I was diagnosed with Crohn’s first 25+ years ago. Then endometriosis 23+ years ago. I have stage 4 endo, meaning it was most recently found fusing my vagina and rectum together. I have had a total hysterectomy, multiple surgeries to remove endometrial tissue throughout my pelvis, and both of my ovaries are now gone. This was discovered after YEARS of constipation (weird for me) and NOTHING worked to resolve it.
Kate is on opioids for chronic pain and her doctors kept telling her the pain medication was the culprit for the constipation, but the reversal medications did nothing. She was hospitalized for nine days for pain and constipation, during which they tried everything. The only fix was to slowly drink colonoscopy prep while getting IV pain meds for the pain it caused.
“I kept asking if it could be a structural or a motility problem, and they kept saying it was the opioids. Colonoscopies have shown my Crohn’s is and has been in remission for years (thanks to Azathioprine!) After the surgery, where they discovered the actual issue (that it was structural), I’ve had zero constipation issues and have been able to finally start coming out of the depression. We are now looking to find a GI doctor who has a better understanding of endometriosis and Crohn’s.”
Kate says the inflammatory process of both diseases mimic each other, and there is no reason to suffer in pain, nor should patients be told they cannot address their pain using the entire toolkit, including opioids, if they allow the patient to become more functional and lead a more fulfilling life.
“Doctors need better education on how systemic both diseases are, and that if Crohn’s symptoms aren’t responding to treatment, they should be worked up for endo. There also needs to be a better understanding that both diseases can be worse than having cancer, as there are no clear protocols, there is little understanding or support, there is little research, and the idea there could be something worse than cancer doesn’t register with most of the general public.”
Lenette: “I found out I had endometriosis when I had a partial hysterectomy to correct iron deficiency anemia. At first, the pain and symptoms all blurred together. It’s taken time for me to be able to distinguish between the two, but sometimes, I’m still unsure what is what. Tracking symptoms helped me distinguish better because I found some symptoms to be cyclical. However, IBD can worsen around your cycle as well and hormones can affect both conditions.”

Lynette recommends women be extremely specific with doctors about their pain. So many symptoms overlap, and she says it can feel two times as bad: bloating, fatigue, mood, etc. All of this can cause pelvic floor tension, and pelvic floor therapy can be life changing.
“It’s also helpful to find community that have both conditions where you can find someone to talk to or learn more about having both. I have found it to be so frustrating to have both because I seem to experience symptoms so much more dramatically than others do at times. Having two conditions that affect the same area and both cause pain and bloating has been so challenging. What helps one condition might not help the other so it can be very trial and error. It has given me a new sense of awareness of my pain and fatigue since I am constantly monitoring to understand which is occurring or if both are the culprit at that time. It’s so frustrating that my IBD is in remission, yet I still experience a lot of symptoms due to my endometriosis.”
She says it can feel like you rarely get a break from pain.
“I try to listen to my body when I’m experiencing a lot of symptoms. I do a lot of deep breathing, stretching, and walking. I also try to listen to my body regarding food. I try to eat nourishing things but also if I’m craving something, I usually eat what I’m craving. If it increases symptoms, I make a note of that. Sometimes my body is OK with certain foods and sometimes it isn’t. I also try to manage stress levels a lot when I’m experiencing symptoms.”
Jessie: “I was diagnosed with Endo and Crohn’s right around the same time at the age of 15. I think my Endo symptoms showed up at first, but they were all diagnosed at once. At the time, the doctors shared no information on any correlation and treated it like two separate issues. As I aged and both progressed, I still struggled to get any acknowledgement from doctors on the two being related; however, once I was diagnosed stage IV Endo and had my last excision + partial hysterectomy, that surgeon said he could see how my condition could be affecting my Crohn’s in the lower colon and perianal area. I had some endo down by the rectum that they removed and there was just a lot of inflammation.”

Jessie says her inflamed uterus (which was adenomyosis) also may have been contributing to overall inflammation in that area as well. She chose to have an excision and partial hysterectomy before her ostomy was reversed, and her perianal symptoms improved so much by not having a period anymore.
“Every time I would get a period, I would experience pain, inflammation, diarrhea, increased urgency, and pressure around that rectal area and my lower abdomen. While I still have my ovaries, not having a period itself every month almost eliminated all those Crohn’s symptoms that would rage around my cycle.”
The Bottom Line
The truth is, not all pain in women with IBD is “just IBD” and continuing to accept that narrative is where too many stories get stuck. Endometriosis is often hiding in plain sight, especially in bodies already labeled as “complicated.” But your body is not confusing, you’re just being asked to connect dots that the healthcare system doesn’t always put together for you.
So, if something feels off, if your symptoms don’t follow the rules, if your pain keeps showing up despite doing “everything right,” do not ignore it. Track it. Name it. Bring it to your care team repeatedly until someone listens.
Because you deserve care that looks at the whole picture. You deserve doctors who are curious, not dismissive. And most of all, you deserve answers, not assumptions. This isn’t about choosing between diagnoses. It’s about recognizing that sometimes, it’s both, and finally getting the care that reflects that reality.

Learn more here
Life With Crohn’s And Endometriosis: An Overlap Of Painful Symptom | EndoFound
Inflammatory Bowel Disease and Endometriosis: Diagnosis and Clinical Characteristics – PMC
Inflammatory Bowel Disease and Endometriosis: Diagnosis and Clinical Characteristics – PubMed\