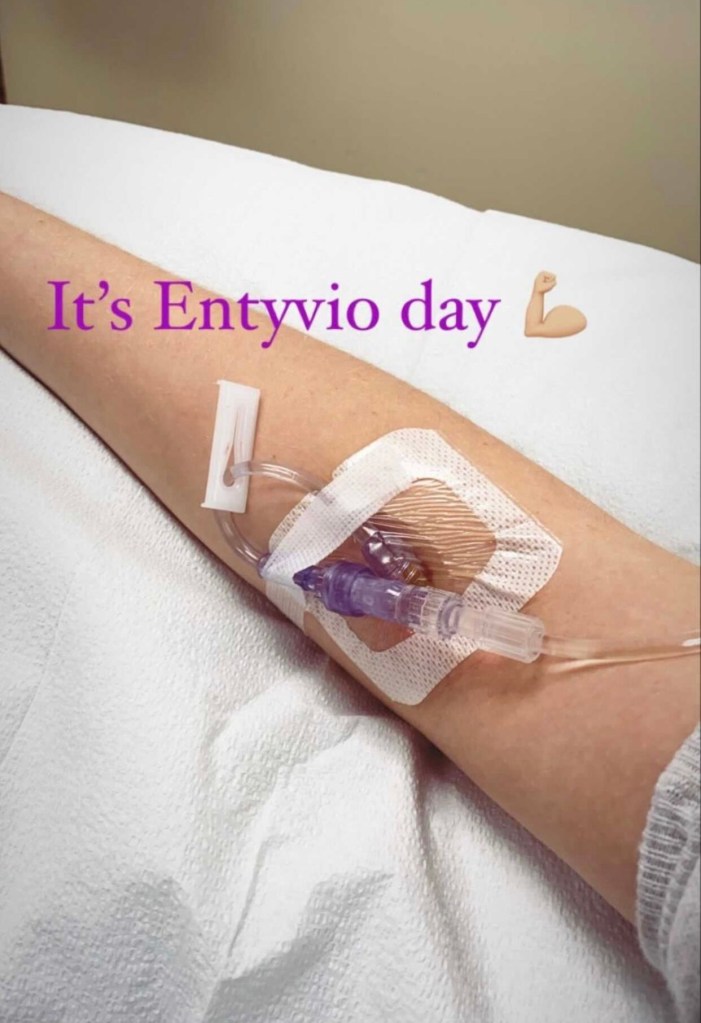
It’s considered the most common surgical procedure for ulcerative colitis patients when medication fails to keep IBD under control. The ileal pouch anal-anastomosis (IPAA) or j-pouch, is created after a surgeon removes your colon and rectum and uses the end of your small intestine to form an internal pouch, which looks like the shape of J.
This week on Lights, Camera, Crohn’s we hear from a colorectal surgeon and IBD patient himself, along with several women with j-pouches about their experience, what they’ve learned along the way, and what they hope others know who are living similar realities.
What does the j-pouch procedure entail?
Before we dig deeper, a short “lesson” on what the j-pouch procedure involves. It’s typically a one, two, or three stage process.
According to the Crohn’s and Colitis Foundation:
- The first surgery removes your colon and rectum and preserves your anus and anal sphincter muscles. The ileum is made into a j-shaped pouch and connected to the top of your anal canal.
- A temporary ileostomy is typically created to give your newly formed pouch a chance to heal. A loop of your small intestine will be pulled through an opening in your abdomen, called a stoma, to allow waste to exit your body into an ostomy bag.
- During this time, you will need to always wear an ostomy bag, and it will need to be emptied several times a day.
- You will have your second surgery eight to 12 weeks later, once the pouch has healed.
- The second surgery will reverse the temporary ileostomy and reconnect your small intestine. Your internal pouch will then collect waste and allow stool to pass through your anus in a bowel movement.
- Some surgeons choose to perform this surgery in just one stage, in which the pouch is created and joined to the anus without a temporary ileostomy. This is done less often than the two-stage procedure because of an increased risk of infection.
This topic resonates with Dr. Stefan D. Holubar, MD, MS, FASCRS, FACS, IBD Surgery Section Chief & Director of Research for the Department of Colorectal Surgery at Cleveland Clinic, for many reasons. He was diagnosed with Crohn’s colitis when he was 7 years old and was on and off steroids (the only treatment at the time) for many years.

“I had learned to live with chronic embarrassing urgent incontinence, as well as being small and skinny, and with a swollen face from the steroids. I was offered an end ileostomy as a teenager (not a J-pouch as it was Crohn’s) and was lucky to get a second opinion with the famous Dr. Daniel Present (RIP) at Mount Sinai. I went on NPO and TPN for one year which helped get me into remission and grow about a foot in one year. Somehow, I made it through college and got into medical school, but it turned out I hadn’t had a colonoscopy in about a decade.”
Over Christmas 1999, Dr. Holubar had a colonoscopy and received a call a few days later while he was skiing that he had colon cancer.
“That same day, the tumor swelled from the biopsies, and I developed a large bowel obstruction. I had emergency subtotal colectomy w ileosigmoid anastomosis without an ileostomy. After chemotherapy and completing medical school, I needed the rectum removed (due to risk of rectal cancer) and underwent a modified 2-stage J-pouch without ileostomy one month before surgical residency. I’ve been great ever since, not perfect as I have had some complications over the years, but great, with three kids, the best job and wife in the world.”
During the second half of medical school, Dr. Holubar was considering going into GI or Medical Oncology and learned that colorectal surgery was a specialty.
“Once I learned Colorectal was a specialty and they are the IBD experts, my future path was set in stone. It’s rare to know that you want to be a colorectal surgeon that early in training. I’m blessed to share my successful story and give patients with complicated IBD like me hope every single day of my life. My experiences have also influenced me to do clinical research to try to change care more broadly and ideally, globally. My IBD history is a source of endless inspiration for our innovative work.”

I asked Dr. Holubar what advice he has for patients who are on the fence about getting a J-pouch. His most important advice—is to seek expertise.
“I would recommend looking for surgeons who specialize in IBD. J-pouch surgery is a niche these days (hence “IBD Surgeons”), and your care team should be expert in taking care of the complications that may develop. A majority (>90%) of patients with a pouch would do it again and/or recommend it to a friend or family member.” (Fazio et al., Annals of Surgery, 2013, PMID: 23299522).
Dr. Holubar wants to highlight a couple important points in terms of this article:
- Only about 10% of people who are deemed candidates for a pouch choose not to have it, for personal reasons such as work, or lifestyle-related reasons such as lack of access to a toilet for many hours at a time, or those who prefer a one-and-done approach (Holubar, Inflamm Bowel Dis, 2009, PMID: 19266572). We have a new article on this, but it has only been published as an abstract so far (Total Proctocolectomy with End-Ileostomy Versus Ileoanal Pouch for Ulcerative Colitis: Who Doesn’t Pouch, And How Do They Do? Dis Colon Rectum 64;5; Meeting AbstractPOD169)
- On the other hand, the overall long-term pouch survival is about 90-95% which is very high (in other words, it works out most of the time, but not always) (Fazio et al., Annals of Surgery, 2013, PMID: 23299522).
- In the current digital era, we are blessed to have support groups on social media and active discussions on #SoMe4IBD. That said, it’s important to know that not everyone who has a pouch – whether the experience is great, or they have complications – is vocal on social media. It’s important to check with your care team to discuss the best treatment options for you.
When it comes to the risk and benefits of having a J-pouch, Dr. Holubar says each patient needs to chart out the pros and cons of end ileostomy (or rarely a continence ileostomy aka Kock pouch) vs. IPAA as the risk-benefit profiles are quite different.
“The main benefit is that a patient can maintain transanal defecation and avoid a permanent ileostomy and care of the ileostomy. An added “benefit” of having a pouch is that you can almost always go back to an ileostomy if it doesn’t work, or you are not satisfied with the function. Going back into the belly is of course with some risk of further surgical complications,” he explained.
The j-pouch patient perspective
Jackie was diagnosed with ulcerative colitis in March 2009. She was 24 years old and had been given a multiple sclerosis diagnosis before that. At the time, her care team was concerned a biologic could set off her MS.
“Less than a year after my diagnosis, I was told that I’d run out of medication options and I’d need to have my colon removed and opted to schedule surgery at that time to work towards a j-pouch,” said Jackie.
Getting acclimated to having an ostomy didn’t come easily. She says her biggest obstacle was getting over her own biases.

“I didn’t know anything about ostomies except from what I read online from other patients at the time and the consensus in the online forums was not good. I was nervous, but I learned almost immediately that I felt better, was healthier, and could do more. After my first surgery, I traveled across the country and hiked through some parks in Oregon. None of that would have been possible before my ostomy. It only took a few experiences like that to realize how much the ostomy had really given me.”
Of course, there’s a learning curve. There’s new terminology to learn, you must find what works on your body, and that can be frustrating.
“I was curious from day one. I knew that I was sent home in the appliance the hospital had set me up with, but I wasn’t convinced that was the best one for me, so I took it upon myself to test lots of brands and products to get the one that worked best for me.”
Jasmine was diagnosed with ulcerative colitis in 2017 when she was 19. She was a freshman in college. Two years later she dealt with a flare she started Entyvio, but the drug failed her shortly thereafter. She switched to Remicade in January 2020 and had the same problem, even after receiving the highest possible dosage every 4 weeks. Her health continued to rapidly decline, and she was hospitalized in March 2020.
“This was the first-time surgical intervention, an ostomy, and a j-pouch were mentioned to me in a real way, however, the doctors continued to say they felt cautiously optimistic Remicade would pull me out of my flare. Throughout these months, I tried a variety of diets including SCD and AIP, visited multiple dieticians and nutritionists, met with natural health doctors, sought out second opinions, and followed a robust supplement regime that was continuously updated by my functional health doctor.”
Despite every effort, by April of 2020, her health was the worst it had been her my entire life. Weighing 105 pounds, she lived in constant, excruciating pain, unable to sleep or eat, too weak to stand in the shower for longer than five short minutes.
“IBD completely ruled my life. When I spoke with my doctors in early May, they told me I had two options: I could try Stelara, the last drug available to me, which my team was 99% sure would not work and would result in emergency surgery since the drug takes months to kick in and provide relief. Otherwise, I could have surgery immediately. My options hardly felt like options when both resulted in the same outcome, just at different times. I opted to have surgery sooner rather than later. If it was inevitable, I wanted to begin the process and start feeling better as soon as possible, rather than continuing to needlessly suffer.”
A few days later, Jasmine met with a surgeon, and less than a week after that appointment (and the morning after her college graduation), she was rolled into the operating room to have my colon removed.

“No life experience prepares you to look down and see an internal organ on the outside of your body. A stoma is far outside the lines of normal human experience, and despite all the preparation in the world, your brain can’t fully process what it will be like until it’s happened. I found the transition to be difficult; while the nurses in the hospital were helpful, the nurses sent to my home barely seemed to know what to do. I had to teach myself how to empty the bag, and at first, it often took me an hour to change the ostomy. However, with time and as my body healed from surgery, I became more confident and able to quickly take care of the ostomy in under five minutes,” said Jasmine.
Even though the physical acclimation was challenging, Jasmine says the mental acclimation was even harder.
“At the time, I was 22 years old and had never in a million years imagined my life to involve a bag of waste attached to my stomach. I felt like I was constantly grieving the life I’d imagined and the life I’d never get to live. The ostomy felt like a reminder of all that had been taken from me that I couldn’t ignore, concrete proof of how different I was from all other 22-year-olds and how far my life had diverged from the normal college experience. I spent many days looking in the mirror and crying at what I saw, struggling to accept the ostomy as the life saver it was. Over time, as I began to regain more freedom and control over my life, eating the food I wanted, sleeping through the night, exercising, and traveling, I slowly began to make peace with the ostomy through the lens of all it enabled me to do.”
Aimee was diagnosed with ulcerative colitis in 2011 when she was 22 years old. She struggled responding to medical intervention and dealt with severe abdominal cramping and high levels of blood in her stool which destroyed her quality of life.

“I had to give up my job, my life, my apartment, my social life and moved back to my hometown to be taken care of by my parents. In one hospital admission 9 months after first symptoms, the surgical team advised I do the ostomy to avoid a tear or rupture to the colon which could lead to emergency surgery or worse, sepsis.”
The ostomy relieved Aimee’s constant cramping and she felt instant relief from her chronic pain. Going into surgery the plan from the start was to do a three-step surgical journey over 12 months that resulted in a j-pouch May 2012.
“There is so much help in the hospital that it was only the day I was leaving that it hit me that this was going to be something that would be hard to get used to. I was 22 and I was embarrassed to tell everyone and conscious of my looks, so there was a vanity piece that was hard to overcome. When I was home, I felt alone. I wanted to manage the bag all by myself, I didn’t allow anyone to see the stoma or my bags or anything. Looking back at my young self, I wish I had let my family and friends in more to help me, I didn’t need to hide it.”
Elissa was initially diagnosed with ulcerative colitis when she was 14 years old, back in 1994 and years later, Crohn’s, in her small intestine. Her diagnosis journey was a difficult one. She was told she was lactose intolerant, had food allergies, IBS, anxiety, and a nervous stomach.
When Elissa was 20, she underwent emergency surgery to remove her colon. She was one of the first patients to participate in a clinical trial for Remicade back in the day. Unfortunately, the medications kept failing her, she became dependent on high doses of steroids, and she had precancerous cells in her colon.
“I was in college at the time and didn’t feel comfortable telling most people. There were a few occurrences of my bag leaking (one especially memorable experience in the middle of a fraternity party), and I was mortified. However, my recovery also highlighted the thoughtfulness and generosity of my best friends and family members who would drive me to the pharmacy to pick up medical supplies, drive me to doctor appointments, even just sit with me and rest. People really come out of the woodwork – sometimes asking for help is the hardest part.”

At times Elissa felt very alone. She wishes she had known the Crohn’s and Colitis Foundation was available, along with support groups. She says, now, there are so many amazing resources available for people in recovery, including the forum j-pouch.org.
Dani was diagnosed with ulcerative colitis in 2005, when she was just 8 years old. She was initially managed on oral medication then switched to biologics and went through Remicade, Humira, Xeljanz, Stelara, and Entyvio.
“I always knew that surgery was on the table, and I felt like I was always buying time until a new medication came out. In January of 2021 I became extremely sick and was admitted to the hospital for IV cyclosporin to try to lessen my immune response. I was ok enough to leave the hospital and was feeling ok for about four days out of the hospital and then I started to become sick again. My surgeon came around a few times to check on me and introduce himself. He said, “I just want you to know that I’m not the scary man with a knife.” At that time, I didn’t know he would be my surgeon. When I started to get sick again after leaving the hospital, I knew that surgery was going to be the next step.”
From then on, Dani met with her GI doctor and Colorectal surgeon (who work together), and they scheduled her for a subtotal colectomy a few weeks later. She began the 3-step surgical process in March 2021.

“It was a huge adjustment. I constantly felt my bag and it felt so foreign to me. At the same time, it gave me an independence that I had never had before. My plan was to go through all 3 j-pouch surgeries to have an ostomy for nine months and then have a j-pouch. I felt confident that I could adjust to an ostomy again if necessary and that I wanted to give a j-pouch a try.”
Dani got her take down surgery J-pouch in December 2021.
The hope of reversing from the start
Jackie: “The plan was to reverse, but I did have a major panic moment a few months before I was supposed to have another surgery. A friend of mine who had started his journey to a -j-pouch around the same time I did, was one step ahead of me in his surgical sequence, and he was having some major problems. I figured the ostomy was the devil I know, better stick with what you know, because I was afraid of what the other side looked like. But I knew myself, and I knew I had to at least try for a reversal, otherwise I’d spend the rest of forever wondering how it would have gone.”
Jasmine: “From the start, the colectomy was presented to me as a step toward the larger goal of getting a j-pouch. I went into the first surgery planning to try the j-pouch.”
Elissa: “I knew the ostomy would be temporary, but I really had no idea what to expect as far as recovery was concerned. My doctors and surgeons did not explain any potential complications. I wish I had known more questions to ask.”
For Elissa, a pouch was created at the time of surgery that removed her colon. Three months later, she had reversal surgery during college spring break – unfortunately, the reversal failed, she caught an infection and ended up in the ICU. The ostomy was placed again for her body to recover from an additional open abdominal surgery. She then went on to have a successful reversal in July of 2000.
Making the decision to go for a j-pouch
Jackie: “I knew that I could have chosen to keep my ostomy, but there was a real sense of “why wouldn’t you get a j-pouch” from the medical team. There was an undertone in what they said and did that insinuated the j-pouch was the more ideal situation and that I should clearly want to go that route. At the time, I was still regularly following most professional medical advice and didn’t really question it. But the option to keep the ostomy was never really discussed and it was always assumed I would reverse it.”
Jasmine: “Because I was young, otherwise healthy, and it had been confirmed many times through testing that I had ulcerative colitis, rather than Crohn’s disease, my doctors said I was a great candidate for j-pouch surgery. In general, my surgeon told me that close to 90% of j-pouch surgeries are successful, and I felt confident trying based on my background and the conversations with my medical team. By the time I’d had surgery, I’d only had ulcerative colitis for three years and had been in remission for two of them. The j-pouch felt like the best avenue for a life as close to normal as possible given the circumstances, and at 22, with (hopefully) a lot of life ahead of me, that sense of normality was important to me.”
How it felt leading up to reversal
Jackie: “I kept reading about all the things that could go wrong and it really freaked me out. I knew people personally who had some complications and it made it seem less like a potential statistic and more like a reality. The reality is that more people do well but are not often talking about it online. At that time there weren’t enough stories about people thriving after j-pouch surgery. I knew what life with the ostomy was like and I knew I could do that. Welcoming another major surgery and another major change just seemed really overwhelming.”
Jackie started the process in March 2010. She unfortunately had a few complications along the way which resulted in more surgeries and a longer sequence to the j-pouch, so her takedown occurred in mid-2012.
Jasmine: “I often worried something would go wrong that would prevent me from getting a j-pouch. Everything that could go wrong had gone wrong for me to even end up 22 and colon-less, and it was hard for me to imagine something could go “right.” I felt very distrustful after the variety of promises made to me by my medical team over the past year that never came to fruition and struggled with cynicism about what might happen. Coupled with all the negativity online about life with a j-pouch, I became very apprehensive about something either going wrong with my surgeries or my j-pouch failing.”
Jasmine’s j-pouch was created in December 2020 with a diverting loop ileostomy and was fully connected in February 2021.
Dani: “I had read about ‘butt burn’ and that when you first get a j-pouch you are going to the bathroom frequently, so I was concerned about that. I had just gotten used to being able to go where I wanted and not worry about the bathroom, and I was concerned that I was going to be putting myself back into a position where I was more limited.”
What j-pouch recovery was like
Jackie: “The takedown was one of the easier surgeries to recover from for me because that was the only thing they were doing in that surgery. Sometimes surgeons combine steps that can make certain parts more difficult to recover from, but for me it was just hooking up the plumbing, which had already been healing internally for months. Despite the complications I had that resulted in more surgery, it gave my body more time to heal, which I think is part of why my j-pouch has been so successful. The hardest part was understanding that the j-pouch can take a year or so to settle, which means you may still have some accidents here or there in the beginning. It wasn’t an immediate magical fix, but over time I learned to understand my j-pouch and to predict its behaviors.”
Jasmine: “J-pouch recovery is an exercise in endurance and mental fortitude, but I didn’t find it as terrifying as it seemed from reading online. From the beginning, I felt like I had far more control than I did with ulcerative colitis. There was almost no urgency, and I could take a minute or two to finish what I was doing before going to the bathroom, rather than having to drop everything and run. Although you do go to the bathroom quite often at the start, having that control makes a huge difference. One of the harder parts of recovery is the acidic stool – waste in the small intestine has more stomach acid in it, which usually gets broken down by the colon, however, without a colon, that acid creates burning on the skin. My skin was constantly raw and sore the first few weeks no matter how much butt cream or fluffy toilet paper I used. Sometimes the burning pain was so bad it would wake me up at night, but now, almost two years out, I rarely have butt burn.”
Aimee: “This was the hardest surgery because it was so long and so much handling of my intestines, my bowel lost function, so I vomited for eight days after my surgery. My doctors considered TPN, but luckily peristalsis started again, and I could eat!
Elissa: “Honestly, recovering from surgeries itself wasn’t too bad, especially after years of IBD flares. Getting rid of my colon provided almost immediate relief. I just had to be patient and let my body heal.”
Dani: “The recovery was the easiest in terms of there weren’t new incision spots. I had to get used to seeing my stoma hole as it closed in naturally and I was still very sore. I also was going to the bathroom frequently and wasn’t sleeping through the night for the first few weeks, which was hard. I was frustrated that I felt like I always needed to be near a bathroom, but that feeling was temporary. “
Pros and Cons of life with a j-pouch
Jackie: “Honestly…it has been so good. I have a total rockstar j-pouch. I eat anything I want (popcorn? yes! all the nuts? yes! spicy food? Yes, please!), I can hold my bowels for hours upon hours. I rarely have any urgency and in general have peace of mind that I can live my life, go where I want, and UC no longer can control that. The cons exist, but for me, they’re small. I’ve had pouchitis a few times, which feels like UC again, but it’s treated with antibiotics and then you’re back on your feet! I have accidents at night maybe once a year. I still use the bathroom more often than a person without IBD, but it’s mostly because I choose to for peace of mind. My digestive tract in no way resembles a normal one, it’s different how everything works now, but it’s not a detriment in my life.”
Jasmine: “My j-pouch has given me a level of freedom I never thought I’d experience with IBD. I don’t currently take any medications, and I don’t worry about flaring or failing a medication the way I would with my colon. Although I know there’s always the possibility of needing medication in the future, I’ve been given more freedom and autonomy over my life than I ever thought possible. I eat what I want when I want. I sleep through the night. I sit through meetings and classes without thinking about the bathroom. I go out with friends, travel, and exercise. For me, the j-pouch has brought me closer to my pre-IBD or deep remission self than anything else, and although there are permanent tradeoffs to having such major surgeries, I don’t regret my decision in the slightest. There is an adjustment phase and a new normal, but that new normal has enabled me to integrate IBD my life, rather than having my life completely consumed by my illness.”
Aimee: “I have had fistulae since at the anastomosis, so they have been tricky to manage, but Humira has been wonderful to me, keeping them at bay and giving me energy to live a full life. I also need to have the scar tissue at the anastomosis stretched surgically every 6 months.”
Elissa: “J-pouch life has been amazing! I was in the bathroom 20+ times a day before my surgeries and felt like a shell of a human being. I’m now 42 and have had my j-pouch for 22 years. I can do pretty much anything a “normal” healthy person can do, just need to take occasional extra precautions like electrolyte replenishment or dealing with occasional pouchitis or Crohn’s flares. (My Crohn’s diagnosis came after my j-pouch surgery).”
Dani: “The first few weeks/months with a j-pouch were tough. Your body needs to figure out how to function with a new man-made organ. I was only comfortable laying down for the first few weeks after the surgery. I really hit a turning point when I was able to start taking Imodium and Metamucil. They were helpful for me in the first few months and now I don’t need them. Three months after my final surgery, I had moved out of my house and was starting a new full-time job. So, the initial discomfort and increase in bowel frequency were very temporary!!”
What j-pouchers wish they knew prior to their reversal
Jackie: “I always say its trading a large set of problems for a smaller, more manageable set of problems. UC was awful for me and ended up being life threatening. It was no way to live. My j-pouch has given me my life back, but it’s not a cure. It’s not perfect. I still have some small problems here and there, but it’s all manageable and in no way resembles life before surgery.”
Jasmine: “It’s hard to find information on j-pouches, and I think many of us turn to the internet to learn about what life with one might be like. I personally found the internet to contain a lot of negative information, making me more fearful going into the surgeries than I would have been had I just listened to my surgeon. I would recommend limiting time spent online and trying to connect with individuals who have j-pouches/ostomies through your doctor or the Crohn’s and Colitis Foundation. These resources provide a more accurate peek into life with a j-pouch and can allow you to ask questions and connect with someone who’s been through the same thing. Most people who are healthy aren’t online complaining about their j-pouch, which skews the sample of information accessible to the rest of us. Whenever I started to feel overwhelmed by everything online, I reminded myself of something a nurse once said to me: the internet is a showcase of the best and the worse situations, more often than not, you’ll end up somewhere in-between.”
Aimee: “I was told this would be the end of treatment and medicine which wasn’t the case. As I had Crohn’s, not UC, I had many more hurdles ahead. Also, a new pouch is new so it’s behavior post op, is not your life. Your body adjusts to the pouch and output goes slower as the post-op weeks go by. The j-pouch is an alternative to an ostomy bag, but has to be adjusted to also. It’s different from having your colon. After a few months though, you will have longer periods between toilet runs and sleep through the night. I go 11pm to 6am with no pooping, which is so much better than those few months post-op when I thought oh dear, this is hard!”
Elissa: “When I had my surgeries, I was 20. No doctors discussed potential fertility issues. My daughter was born via IVF 9 years ago, though all additional efforts have failed. This is something I wish I had known about – I always wanted kids and would have frozen my eggs. Obviously, every person is different. Also, I still go to the bathroom 6-7 times a day. This is apparently normal (though again, everyone has different experiences).”
Dani: “I can eat salad for dinner with no problem!”
Advice for ostomates on the fence about going for a j-pouch
Jackie: “If you feel healthy and strong both physically and mentally, I would say, try it. I know it’s more complicated than giving a new restaurant a try, but I knew that I’d always have wondered. I knew on the bad days I would have idolized a life with a j-pouch, and I needed to know that it either would or wouldn’t work. I felt like the worst-case scenario was that my j-pouch would fail, and I’d return to an ostomy, which I already knew I could do, and I liked those odds.”
Jasmine: “I think it’s a personal decision dependent on the history and circumstances of each person’s illness. Going through the j-pouch surgeries means additional time spent in the hospital and recovering, which is worth it for some, but not others. Although I can share my experiences, everyone’s body is different, and you can’t always predict how someone else will respond. I think the best thing to do is find a colorectal surgeon skilled in these procedures and discuss whether they think you’re a viable candidate. Finding a skilled surgeon is the best way to hedge against future problems and increase chances of success. Beyond that, I would advise talking to as many people as possible with a j-pouch and permanent ostomy, to get questions answered and hear the pros and cons of each route. Having this information should help you feel more confident in your decision, and if you’re still undecided, you can always put off the decision until you’re ready.”
Aimee: “Tell them to get support, don’t expect instant results, give yourself time to adjust to yet another way of going to the toilet…reach out to the online community.”
Dani: “I think this is a very personal decision and there is validity to both sides. An important thing for me was to remember that people are more likely to write online if they have a bad outcome rather than a good outcome. Everyone’s instinct is to research things online and at some point, I felt like reading everything (both good and bad) was too overwhelming.”
Post-op expectations with a j-pouch
Like any surgery, recovery takes time and patience. The Crohn’s and Colitis Foundation shares the following on their website:
- Some patients may experience an increased number of bowel movements, sometimes up to 12 times per day. This will typically decrease over time.
- Some male patients may experience sexual dysfunction as a result of nerve damage.
- Some female patients may develop scar tissue that surrounds their ovaries and fallopian tubes, which may lead to infertility.
- Both men and women should discuss sexual function with their surgeon and ask when it is safe to resume sexual activity.
- Ask your healthcare providers what supplies you may need at home, especially if you have a temporary ileostomy.
- Your healthcare team will advise you on how to manage your temporary ostomy and how to keep it clean.
Final Thoughts
Jackie: “This is a weird one, but I had to use brain power the first time I had to poop after my takedown. It had been almost 2 years since I had used my butt, and I had to really think about how to use those muscles again. It was a little funny at the time.”
Jasmine: “In terms of recovery, the most important thing to remember is j-pouch surgery completely alters one of the body’s major systems and adjusting takes significant time. Recovery doesn’t happen overnight, and it can feel frustrating. I tried to give my body some grace and the time it needed to heal, while reminding myself that life with a j-pouch during the first few week’s post-op isn’t indicative of what living with a j-pouch will be like long-term.”
Aimee: “It’s a journey. I have a few good months, a few bad months. Part of me knows that quality of life could be better with an ostomy, but I’m not ready to say goodbye to my pouch yet. I have been unlucky with the scar tissue, but those small procedures are like going to the dentist for me, I’m so used to them.”
Elissa: “Do it! Healing takes time, but you will feel like a new person. Life is too short to be in pain all the time. So many improvements have happened over the past 10-15 years and awareness is absolutely the key. “
Dr. Holubar wants to remind patients, “The J-pouch cannot save your life – it is a lifestyle operation like cosmetic surgery in some way. Overall quality of life is excellent with both a pouch and with a permanent end ileostomy. Finally, we should think of surgery as an excellent “medical” therapy in patients suffering from colitis despite modern medicines. One of my expressions is that a good ileostomy (or pouch) is better than a bad colon, rectum, or anus (and a good ileostomy is better than a bad pouch). The great news is you cannot make a wrong choice.”