When it comes to the biologic, Humira (adalimumab), I am somewhat of an OG. I’ve taken Humira to manage and treat my Crohn’s disease since July 2008. We go wayyy back. Since my first loading dose 14 years ago, I’ve had hospitalizations, had bowel resection surgery, gotten engaged and married, traveled, worked full time, had three children, breastfed, been a stay-at-home mom…the list goes on. I’ll never forget how overwhelming it felt when I was lying in a hospital bed with an abscess the size of a tennis ball in my small intestine and when my GI at the time told me “It was time to break out the big guns.” The big guns being biologics.

My mom and I were upset. We were frantic. We were Googling. We were fearful of what this would mean for my childbearing years. I couldn’t fathom the thought of giving myself injections or getting infusions. My world came to a standstill. In that moment, I would have given anything to have a resource like this. An article that outlines patient experiences across the board. The good, the bad, the ugly. I write these articles, so you feel empowered and educated when you take the plunge or when you are forced to switch medications because another biologic fails you. I write these articles, so you feel confident in making informed choices and realize that the “big guns” are oftentimes necessary and not as scary as they sound.
As you read this article and others like it, please remember these are individual experiences. Just because one person had a terrible response or reaction doesn’t mean you will. Just because I haven’t had any side effects and have been able to stay on Humira for more than 14 years, doesn’t mean the same will be the case for you. Use these experiences to level your expectations and have a better grasp of what it’s like to be someone with IBD on a biologic drug and make an informed choice with your gastroenterologist.
If you haven’t done so already, be sure to check out previous Patient Experience articles I’ve shared on Lights, Camera, Crohn’s about:
The Shift to Citrate-free Humira
For those who are “new” to Humira, those who are preparing to do their loading dose, or those who aren’t familiar with the drug—in the United States a new and MUCH improved Citrate-free formula came to market for pediatrics and adults in late summer/early fall 2018. I did my first Citrate-free or as many of us call them, “pain free” injection in September 2018 while pregnant with my second child. If you’ve been on Humira for a long time like me or tried it prior to that time, you know how painful the injections used to be and how much easier they are now. It’s a gamechanger. The loading dose used to be four injections—all in the same sitting that felt like liquid fire were going through your leg or abdomen. Fast forward to 2018, not only is the needle gauge smaller, but the formula no longer stings. Click here to watch the video of me experiencing Citrate-free Humira for the first time while pregnant.

I went from dreading my injections (even a decade in) to doing injections on my couch and smiling ear to ear while my kids watch me because I feel next to nothing. This is important context for this article. Some of the experiences you will hear will be from people who never had a chance to experience Citrate-free Humira, and others who say the shot is “easy” to do most likely started or were switched over to the pain-free version. This change in the formula has been an incredible win for anyone on Humira in the United States. The loading dose not only won’t hurt but is only two injections now versus the original four. The challenge is getting used to the mechanics of doing a self-injection and getting into the right headspace each time you’re due for a dose. Regardless of whether it hurts or not, you are still injecting a heavy-duty medication, which suppresses your immune system, into your body. I’m often asked if I get “sicker” being immunocompromised and being a mom of little ones—my answer to that is no. I am mindful of washing my hands and not eating or drinking off anyone. My GI has me do “safety labs” every three months to monitor my bloodwork, along with an annual colonoscopy.
Debbie: “I was on Humira for four years. I responded well at first and liked the ease of doing injections myself. The Citrate-free version was much better and less painful than the original version. I unfortunately ended up developing antibodies and have been switched to Stelara. I didn’t have any side effects with Humira other than some itchiness at the injection site. Ice helped a lot with that.”
Melanie: “After a reaction to Remicade, I was so anxious to try another biologic. This was in 2009 and Humira hurt so much. I had a massive panic attack trying to do the loading dose of the original version. I was 19 at the time. I couldn’t continue with it. Now, I’m on Cimzia, but had to take a mental health break from biologics for a few years.”
Brad: “I started Humira back in March of this year. It’s been a complete gamechanger for me. Humira has me in clinical remission as of my last colonoscopy. I don’t have much reaction to it. Sometimes, the injection can hurt a little bit, but usually not at all. I’m shocked at how easy it’s been. I was originally very nervous about starting an injectable.”
Jenn: “Humira was traumatizing. It took well over a year for me to self-inject without stressing and crying beforehand as the injection hurt so much. While it did provide relief from symptoms for a while, the reaction I ended up getting was significant, and impacted my ability to live normally. So not only had my Crohn’s symptoms returned, but they were also joined by additional symptoms caused from a reaction I was having to the medication. I will never not be a proponent of taking meds as they do help, but I will also never forget the experiences I lived due to them.”
Natasha: “I was in the pediatric trials for Humira. I don’t remember it doing much, but almost 15 years later, I’m still traumatized by the trigger mechanism and feel the phantom pains in my legs from doing them for so long. Anytime a new medication it brought up and it’s a shot, I ask if there are self-administered options vs the auto injector. The PTSD is bad.”
**It should be noted Humira can be administered with an auto-injector pen (where you press down on a button and there’s a clicking sound) or with a syringe where you draw up the medication. I have only used the auto-injector and prefer the ease of it, but it’s all personal preference and what you are comfortable with.**
A mixed bag of experiences
Sofia is now on Stelara after having surgery to remove some of her bowel. When she thinks back to her time on Humira, it’s not a pleasant memory.
“I experienced all the normal flare up symptoms while taking Humira and gained a lot of weight. I just remember my self-esteem plummeted as well as my hopes for remission.”
Kathy: “I was on Remicade, but I’ve been on Humira now for five years and have had great results with minimal side effects.”
Kaitlyn: “I have been on Humira for a few months to treat my Crohn’s disease and Hidradenitis Supprativa and it has been life-changing. My Crohn’s is in microbial remission, and I no longer have to get weekly, painful steroid injections for my HS.”
Jessica: “I’ve been on Humira for four years and my last colonoscopy showed there was mucosal healing and no active Crohn’s. I inject every 14 days and it has gotten easier, especially when I inject and tell myself that it is healing my body. Then, I don’t feel the shot. I’m very thankful for it!”
Myisha was on Humira for a year and then had a major allergic reaction.
“The last injection I gave myself, my face, lips, and mouth swelled up and I got lightheaded. My husband immediately called my GI and I had to be given an EPI pen along with 4 Benadryl intravenously after being rushed to the emergency room. I experienced hypersensitivity anaphylaxis and angioneurotic edema.”
Keyla: “When I was on Humira, it made me lose my hair. I felt terrible on it, and I never noticed much improvement with my IBD.”
Danielle has struggled to find a biologic that manages her disease. Both Humira and Entyvio failed her. She’s now on Stelara.
“I was on Humira for three months in 2021. It worked amazing right off the bat, then suddenly I had no response whatsoever. The injections were quite traumatic for me as I had one injection needle fall apart as I was giving the injection.”
Sarah: “Humira has improved my life and helped manage my Crohn’s symptoms and allowed me to eat a wider variety of foods then when on previous medications. However, there have been some compromises on my part. I’ve dealt with some bad injection site reactions that have caused me to have to take allergy medication prior to administering it to help manage the reaction. I’ve also experienced severe sinus congestion and uveitis that I did not have prior to taking Humira. I’ve lost some sense of smell due to how bad my congestion can get, and I can’t touch or rub my eyes without risking a flare up of uveitis. Overall, I would say that it has been worth taking Humira. I’ve learned to manage my side effects and have gotten over my fear or self-injection.”
Catie: “My experience with Humira was good at the beginning. The medicine helped me achieve remission. The injections were always so painful no matter what tricks I tried. I ended up getting drug-induced lupus from Humira, so I went off the drug. The drug-induced lupus took more than a year to recover from—it was awful.”
Hayley: “I was on Humira for a year and was doing great on it, practically in remission. Unfortunately, I developed psoriasis (which I’ve been told is a rare allergic reaction to the drug itself). My sister who has Crohn’s was also on Humira and had the same reaction. I wish I could’ve stayed on it longer because it was easy and helped me so much, but unfortunately, I had to come off it. It was my first biologic and gave me a lot of hope!”
Krista: “I was on Humira for about 6 months. It was working great—other than extremely painful injector pen that I dreaded using every month. I started to develop scaly patches on my legs, back, stomach, and scalp. My hair started falling out where the scaly patches came up on my scalp. My dermatologist thought I had biologic-induced psoriasis, so I stopped taking it. My biopsies came back negative for psoriasis, but I still ended up switching medications.”
Melissa: “I was on Humira in the past. It didn’t work for me and caused me so many issues. My body itched so badly while on it. I would scratch sores on my body from it. My joints ached all the time. And on top of it, my ulcerative colitis got worse while on it.”
Adriana: “I was on Humira for a year. I did weekly injections, but they wanted to increase my dosage to two injections. For me, it didn’t work (as with a lot of drugs I was on), but out of all of them, it worked best at making me feel better. I don’t remember having too many side effects from Humira besides slight bruising around the injection site, but definitely worth a try!”
Ellie: “I started Humira in 2019 after a four-month bout with steroids. I went into remission a month later after only two injections. I have remained in remission ever since.”
Dana: “I was on Humira for around 2 years. It put me into remission, and I was doing very well, but then I started to have Crohn’s symptoms. My doctor thought about increasing the frequency of my dosage, but my blood levels were adequate, and she didn’t want them to become too elevated with an increase in dosage. I also developed severe psoriasis on my scalp as a side effect. I ended up flaring and having to stop Humira to try something else.”
Jessica: “Humira has been great for me! Really no side effects. I did have to increase my dose to weekly because I metabolize medication too quickly.”
Phil: “I had a small bowel resection in 2004 and after a 10-year remission, my Crohn’s became active again. I was put on Humira, and it was amazing for about 7 years with a few side effects, biggest one being hypersensitivity to the sun. I miss being on Humira because it also helped my joint pain and psoriasis.”
Stacey: “Humira was my final effort to save my large intestine and felt pretty good on it! Aside from horrid cystic bacne, which isn’t listed as a documented side effect (but I swear there was an association there!), I had no side effects, and I felt great on Humira! It gave me a quality of life! I was on Humira when I made the hard choice to have a total colectomy, and the disease had spread since my scope four months prior. Goes to show that symptoms don’t always correlate with inflammation. But I’m grateful for my experience and the opportunity to safely take Humira.”
Pregnancy and motherhood with Humira
As an IBD mom of three, I stayed on Humira until 39 weeks pregnant with my oldest, and 37 weeks with my second and third child. I had scheduled c-sections with all three, so I was able to coordinate my injection schedule with my GI ahead of time. I breastfed my second child for about 6 months and supplemented and just finished exclusively breastfeeding my 14-month-old—all while on Humira. I have three, perfectly healthy children and had flawless, Crohn’s-free pregnancies. I also did not experience post-partum flares and I credit that to the fact I stayed on my medication and picked it right back up the day we brought the babies home from the hospital.

Check out these helpful resources for pregnancy and biologics and have long-term research that shows the safety and efficacy of staying on Humira through the entire family planning process, pregnancy, and beyond:
Dani: “My experience with Humira has been wonderful. I’ve been taking Humira for two years. The nurse ambassadors are so nice and helpful. I was nervous about the injections, but they really are so easy and don’t hurt. Humira has helped me to feel the best I’ve felt since my Crohn’s diagnosis 4.5 years ago. I stayed on Humira through my pregnancy, and I had no Crohn’s related issues during or after. It’s been a life-changer. Most days, I almost forget I have a chronic illness. I’m praying things stay like this, at least until we have another child.”
Stephanie: “I have been on Humira since 2016. I was diagnosed with ulcerative colitis postpartum after my first baby in 2015 and was incredibly sick. I had multiple blood transfusions, tons of steroids, etc. I had some reactions to Humira when I started taking it (skin rashes and almost withdrawal-like symptoms) before the two weeks was over, which almost presented itself like lupus, so I was put on weekly injections and have been doing that ever since. After I was put on Humira, it was a lifesaver. I felt the best I had in forever. Since having my second child in 2019, it’s been more up and down. At my next colonoscopy, we will look to see if I have inflammation still and if I do, I will go off Humira (which is so scary to me) and try something new.”
Katie: “I have been on Humira for 7 months. I was completely terrified to be on Humira, but I was so sick, and knew I needed to do something for not only myself, but my husband and my kids. Humira has gotten me back to the point of feeling back to my normal self. The only side effect I noticed for the first few injections is I would feel absolutely exhausted that next night. It’s super quick and I get on with life as usual!”
Sarah: “I have been on Humira for a little over a year now. I was on it while pregnant with my son. It was an easy process. But now that I’m 4 months postpartum, I am experiencing some weird side effects. My liver levels are elevated, and I am getting symptoms back. My GI and rheumatologist are thinking of moving me to once a week or adding another medication. I am fearful they will switch me off or add things and I won’t be able to breastfeed any longer. Humira has been wonderful, and I am just nervous my body has begun to build antibodies against it.”
Cece: “I have struggled with my ulcerative colitis symptoms on and off since I was 19. At 36 years old, after trying 3 years to get pregnant, I had a colonoscopy that revealed active inflammation. That was what finally pushed me to get on Humira. My symptoms settled down and luckily, I’ve been in remission and feeling great ulcerative colitis-wise through IVF, pregnancy, and breastfeeding.”
The Pediatric patient point of view
Emily is a 13-year-old who has been on Humira for three years. She says Humira has done a lot to help her get Crohn’s under control.
“Doing injections myself has helped. It feels better to “be in control” of giving yourself the shot. I’ve been having less stomach pains and less joint pains from Humira. My joint pain and stomach aches used to be really bad. I used to cry myself asleep at night because how bad the pain was for both my joints and stomach. Now that rarely happens. Yes, I still get joint pains, but not to the point where I start crying. I get a little tired after the shot, but it helps me a lot. So many positives.”
Celia is 15-years-old and started Humira in October 2021. About two months after her initial loading dose, she started to notice less bowel movements, but still had urgency and abdominal cramping. Her GI decided to increase her dose to 80 mg since her inflammation markers were elevated and she was flaring. (Typically, we are put on 40 mg injections, twice a month).
“I feel better! I still have my bad days and have had minor issues. I’m hopeful that this will be the medicine to get me into remission! On the mental side of things, I have struggled with injection anxiety. I have never been afraid of needles, and I’m still not, but I overthink every injection. That has been my greatest struggle on Humira, but I’m hopeful over time I’ll overcome it!”
Cindy’s 8-year-old daughter is on Humira. She says the various worries and challenges all give way in the end to gratitude.
“Humira is saving my daughter’s life and giving her a tremendous quality of life. Thirty years ago, an 8-year-old would have had such a different trajectory my she is experiencing and hopefully will continue to have. I love science.”
Struggles with access to Humira
Regardless of the biologic you are on, dealing with insurance, prior authorizations, and specialty pharmacies can make access to drugs like Humira a challenge. AbbVie (the maker of Humira) offers several programs to help streamline the process and take some of the burden off patients.

Once you enroll in Humira Complete, you are connected with a Nurse Ambassador who will speak with you directly (and even do in-person visits) to help you gain confidence and understanding about everything from administering your medication to any side effects you may be dealing with. Humira Complete offers a Patient Savings Card and Prescription rebates, and offers injection training through videos, an App to help you stay on track, and 24/7 availability should you need to reach someone. The phone number for Humira Complete is 1-800-4HUMIRA (1-800-448-6472).
Even though Humira Complete exists and has helped me many times, there are still many patients dealing with access issues or completely unaware of the fact that the programs and savings are available:
Emily: “I have been on Humira since October of last year and it has been both great and horrible for me. Remicade stopped working for me after 5 years and Humira was able to help calm down the flare I had been experiencing. I learned with time that at home injections weren’t something to fear. Humira is very convenient. Humira came with large bills and a battle with insurance and Accredo pharmacy. Every month, unnecessary stress had been added to my already full college schedule. In between classes I found myself calling multiple people to make sure my medication was going to arrive on time and that it didn’t cost me $4,000 each time. I’ve had issues almost every single time I refill my medicine. It almost makes me want to switch medicine just so I don’t have to deal with it, which is unfortunate because the medicine itself helps me.”
Sydney: “I just came off Humira. It worked great until it didn’t anymore. The formula changed a few years ago, which made it a lot more tolerable, but for a very tiny human, the auto injector caused some atrocious bruises. I ended up having to use syringes because of the bruising. It was a fight with insurance almost every time I needed a re-fill. The medication was good, but the stress trying to get it was almost not worth it. I only reached remission for about a year on it and then my body figured it out.”
Sam: “I have been on Humira for five years. I would say the issues aren’t the drug itself. Insurance companies make it so hard to get access. Ordering my medication from a specialty pharmacy is the worst.”
Christie: “I have been on Humira for three years after being diagnosed with ulcerative colitis in early 2019. The decision to begin taking Humira was a tough one, but I wanted to try anything to reach remission. While I have had a few insurance hiccups here and there, my experience with Humira has been great. I am enrolled in the Humira Complete Program, where I can track my injections and a nurse ambassador calls me once a month to check in. The resources AbbVie offers are incredibly helpful. Overall, I credit Humira for getting me into symptomatic and endoscopic remission.”
Final thoughts
All in all, you must always weigh the risks versus the benefits when determining a treatment plan with your physician, regardless of the medication. I personally have not dealt with side effects and have relied on Humira to help me maintain my remission and feel my best so I can be present for my family. What started out as a shocking change in my life, is now just part of my routine. Be patient with yourself and whether the injection hurts or not, reward yourself after. I usually enjoy some ice cream while watching reality TV. Giving yourself an injection isn’t easy, treat yourself to something for being a compliant patient who is doing all you can to help treat an unpredictable and complicated disease. And most importantly, remember you are not alone in your fears, your struggles, and your worries.

























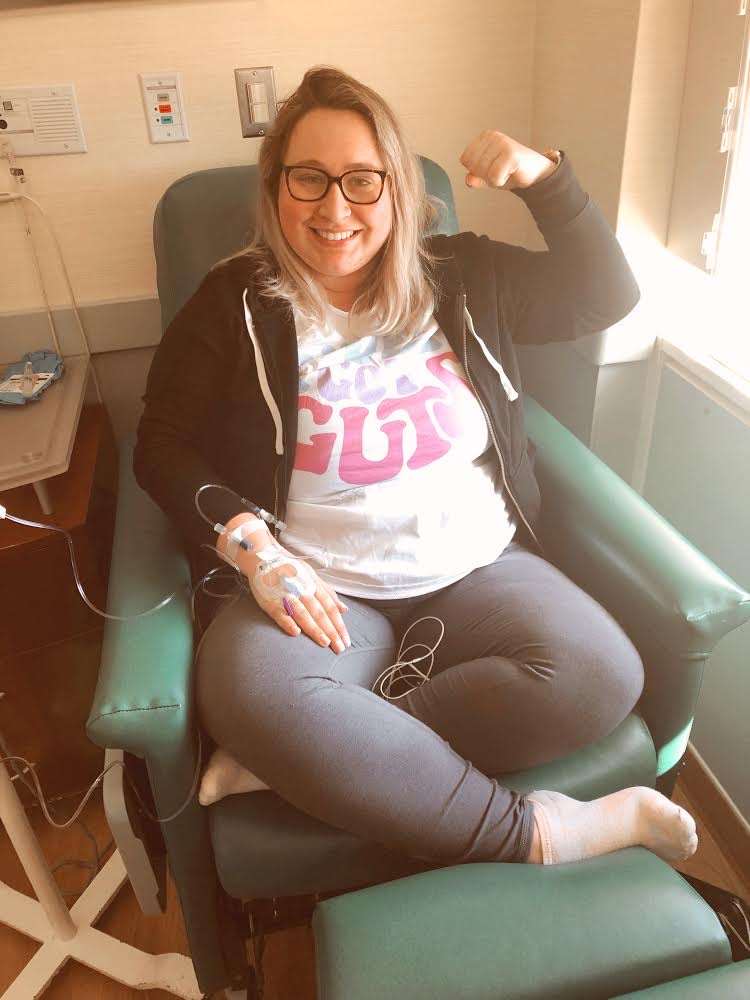








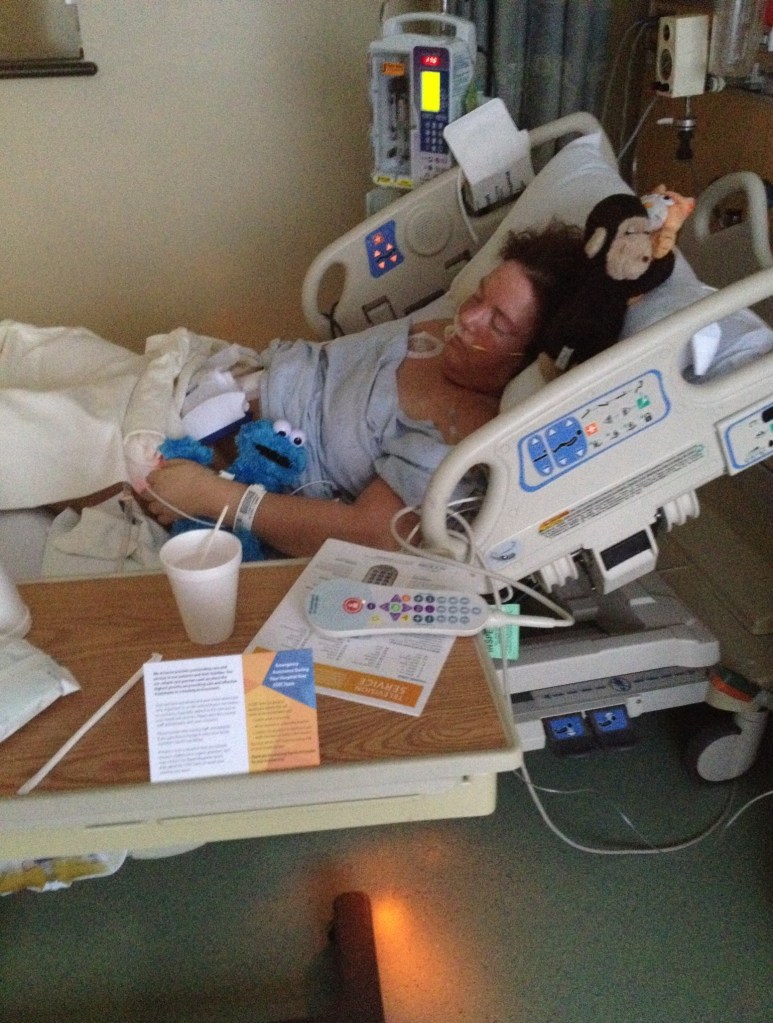








 She has ulcerative colitis and I have Crohn’s. She is 24 and I’m 36. But, our lookout on life and our interest in bringing comfort and serving as a positive voice for the community is the same.
She has ulcerative colitis and I have Crohn’s. She is 24 and I’m 36. But, our lookout on life and our interest in bringing comfort and serving as a positive voice for the community is the same. So not only does she have her own personal patient experience, but she’s been a part of a family unit who’s dealt with the ups and downs her whole life. It was emotional for me as an IBD mom, to hear firsthand from a 20-something about what it was like to not only grow up with a mom who has Crohn’s, but later be diagnosed with IBD herself.
So not only does she have her own personal patient experience, but she’s been a part of a family unit who’s dealt with the ups and downs her whole life. It was emotional for me as an IBD mom, to hear firsthand from a 20-something about what it was like to not only grow up with a mom who has Crohn’s, but later be diagnosed with IBD herself. If you’re looking to follow someone who is sure to lift your spirits and make you feel empowered, she’s your girl. When I chatted with her on the phone, I told her how much I look up to her for her advocacy work, despite being 12 years older!
If you’re looking to follow someone who is sure to lift your spirits and make you feel empowered, she’s your girl. When I chatted with her on the phone, I told her how much I look up to her for her advocacy work, despite being 12 years older!