In 2016, Nick Zecchino was living the dream. After years of relentless dedication, he signed a Division I football scholarship to the University of Connecticut. For a young athlete who had poured his heart, body, and soul into the sport he loved, it was validation that every sacrifice had been worth it.
“I was on top of the world,” Nick recalls. “It was the proudest day of my life to that point. Then, one month later my health started to decline out of nowhere. It was scary, there were a lot of questions and uncertainties with what my future was going to hold.”

This week on Lights, Camera, Crohn’s a look at Nick’s remarkable journey and his comeback story both on and off the football field that left me in awe.
When a Dream Collides with a Diagnosis
Like many of us, Nick’s health issues blindsided him out of nowhere. He lost his appetite. Crushing fatigue set in. Blood appeared consistently in his stool, and his bowel movements increased dramatically. In March 2016, a colonoscopy confirmed what he had never even heard of before: ulcerative colitis.
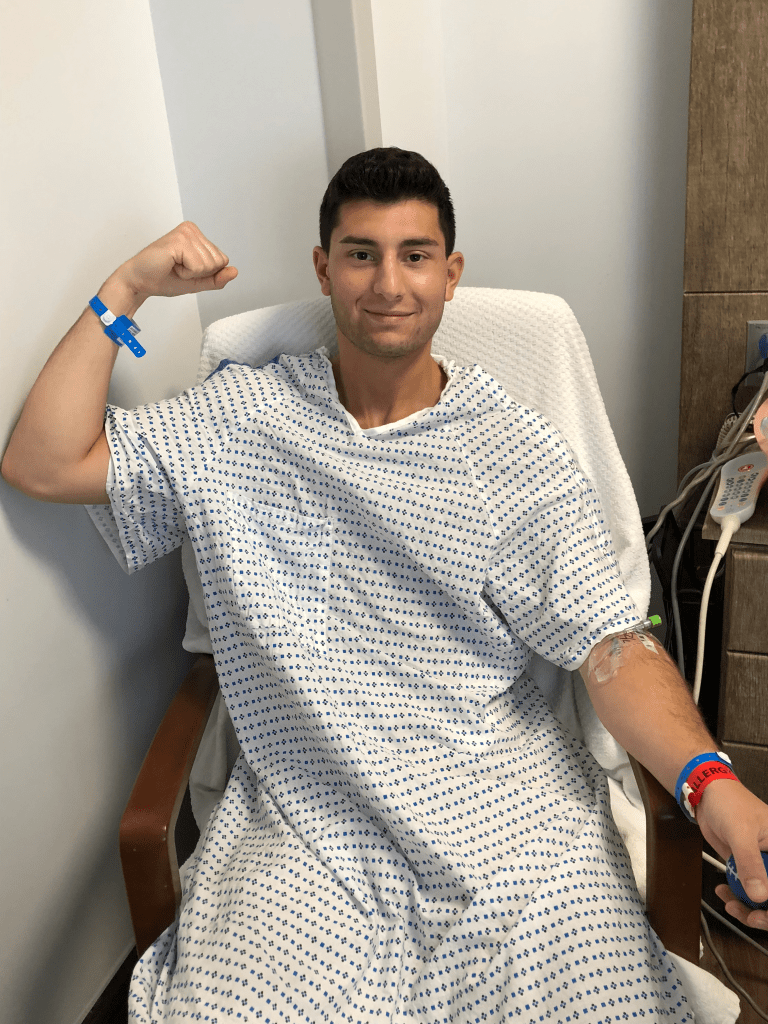
At first, Nick assumed it would be manageable. Get it under control. Heal up. Be ready for UConn by June.
“I didn’t know the long road ahead,” he says.
Weeks turned into months, and instead of improving, his symptoms worsened. During his senior year of high school, Nick missed most of his baseball season due to a constant flare. Maintaining weight and building muscle, which are essential for a college football player, became nearly impossible. By April, the fear crept in: What if this costs me football?
Playing Through the Unthinkable at UConn
Nick arrived on campus determined to push through. But ulcerative colitis never truly loosened its grip.
From the first game of his freshman season to the last, his health declined sharply. Between September and November alone, during his first college football season, Nick lost more than 50 pounds! By the final game, he weighed just 145 pounds and looked visibly ill. He used the bathroom 20 to 25 times a day, often passing only blood and mucus.
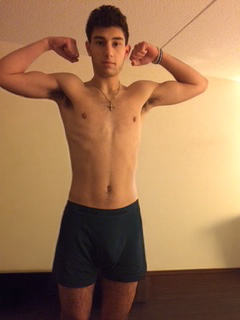
“There really wasn’t any managing it at that point,” Nick says. “I just had to deal with it and the consequences.”
He tried to hide his illness from coaches and teammates, unwilling to show vulnerability or weakness. He timed bathroom breaks to the last possible minute before kickoff, rushed off at halftime, and avoided eating on game days altogether. Even then, the urgency never stopped.
Years of Medications and No Relief
Nick’s treatment history reads like a roadmap of severe disease. After initially trying mesalamine and Lialda, his doctors escalated to stronger therapies as his condition worsened. Over time, he was on Remicade, Humira, Entyvio, 6-MP, prednisone, and antibiotics like Cipro. He even tried multiple biologics still in clinical trials for ulcerative colitis.
Nothing worked to wrangle his IBD under control.
At one point, doctors administered the maximum dose of Remicade possible, at the shortest interval allowed. It still wasn’t enough.
A Turning Point
Eventually, Nick’s dad made the hardest call of his life.
“My dad picked me up from UConn because I couldn’t go on like that anymore.”
A few days later, they were sitting in a doctor office at Mount Sinai in New York with Dr. Arthur Kornbluth, an IBD specialist who would change the course of Nick’s life.
“Going to Mount Sinai saved my life,” Nick says simply.
Dr. Kornbluth tried everything. Every possible medical “trick in the book” to try and get Nick into clinical remission. But despite his efforts, Nick couldn’t achieve lasting remission. Finally, they faced the reality neither wanted to confront: surgery.
“It was terrifying,” Nick admits. “But it was the only way I could get my life back and maybe still have a chance to play football again after my future was put on hold for over two years. Making the decision to go to Mount Sinai and get surgery completely changed the trajectory of my life. It will always be one of the best decisions I’ve ever made.”
Three Surgeries. One Unbreakable Goal.
Nick had a total colectomy (which removed his entire colon and gave him a temporary colostomy bag, followed by Takedown surgery and a J-pouch). After the three surgeries in six months, Nick finally began to feel like himself again. In January 2019, he returned to the gym for the first time.


He was weak. Deconditioned. A shell of the athlete he once was. But his motivation never wavered.
“Football was my one and only motivation,” he says. “I spent nights in the hospital bed thinking about how I could get back on the field.”
By June 2019, Nick arrived at Purdue University. At this point, he was not just healthier, but also confident that his dream was no longer out of reach.
A Second Chance at Everything
Walking onto Purdue’s campus felt surreal. Nick felt like a freshman again, even though he wasn’t. In many ways, it was a new life.

“I was just so grateful,” he says. “I had a completely different outlook than anyone else my age.”
When game day arrived, the nerves hit harder than they ever had before. But the moment he took his first snap, they vanished.
“I felt like myself again,” Nick says. “It was one of the best feelings in the world.”

From that point forward, confidence replaced fear. He had already survived more than most people ever would.
Life After UC—and Living Medication-Free
During his four years at Purdue, Nick dealt with recurring pouchitis every couple of months. Antibiotics like Cipro helped, but he grew tired of relying on medication.
Determined to find another way, Nick dove into research on gut health, inflammation, and natural support. Supplements like L-glutamine made a noticeable difference. Eventually, the pouchitis stopped coming back.

One day, his dad noticed the growing lineup of supplements on the kitchen counter.
“If this works so well for you,” his dad asked, “why not create something that could help other people too?”
That conversation sparked the creation of Carna Nutrition and its flagship product, GUT R3BU1LD—a gut health formula inspired by Nick’s own journey.
The name Carna comes from Roman mythology: the goddess of health, vitality, and protection of the internal organs, while helping with digestion.


“I created the full spectrum formula of our product with the help of a health & wellness professional that has been in the industry for 25+ years,” explains Nick. “We also used the access to the manufacturers’ scientists that they have in-house to help us understand the way that the pharmaceutical grade and clinically studied dosages of the ingredients that we have in the product all work together synergistically in a beneficial way for every major gut healing pathway during digestive stress.”
“He Was on His Death Bed. It’s Incredible What He Did.”
Nick’s comeback left a lasting impression on everyone who witnessed it, including his football coaches.
Former UConn head coach and Purdue defensive coordinator and linebackers coach, Bob Diaco, recalls:
“I remember watching him and trying to figure out how to stop it. My wife hadn’t seen him for a few months, and she was distraught. He was on his death bed for real. It was bad. It’s incredible what he did.”
“He’s the kind of kid that makes you better,” Diaco continued. “He’s been the underdog at every turn. He always comes out on top. He’s always making an impact on the people around him in a positive way.”
A Message to His Younger Self and to Young Athletes Today
If Nick could speak to his 2016 self, he knows exactly what he’d say:
“Your journey isn’t going to look anything like you imagine, but it’s going to be the most rewarding path for you. Trust it.”
And for young athletes with IBD who are scared their diagnosis might end their dreams?

“Your diagnosis is not the end of your story,” Nick says. “You’re allowed to struggle. You’re allowed to take time to heal. But don’t lose hope. Most of the battle is mental. Stay strong, stay supported, and keep chasing your dreams.”
Where to Find Nick and Carna Nutrition
- Carna Nutrition Website
- Instagram: @nickzecchino/@carnanutrition
- Facebook: Carna Nutrition
Nick’s story is a reminder that even when IBD takes everything, it doesn’t get the final word. Sometimes, it forges something stronger than before. Whether you’re a young person living with IBD or a caregiver worried about what the future will hold for your child, I hope Nick’s incredible story of resilience serves as inspiration to show all that’s possible despite the difficult diagnosis of IBD. I found it interesting that Nick wouldn’t trade all he’s endured to be where he is today, as I always say the same. As time passes and hindsight is 20/20 so many of us experience a transformation that shapes who we are today, all because of the struggles that took us to get here.




















